East Asian Arch Psychiatry 2012;22:141-5
ORIGINAL ARTICLE
从受害者角度分析精神病住院患者的暴力行为
Dr Dhanya Raveendranathan, MD, Department of Psychiatry, National Institute of Mental Health and Neurosciences (NIMHANS), Bangalore, India.
Prof. Prabha S. Chandra, MD, FRCPsych, Department of Psychiatry, National Institute of Mental Health and Neurosciences (NIMHANS), Bangalore, India.
Prof. Santosh K. Chaturvedi, MD, FRCPsych, Department of Psychiatry, National Institute of Mental Health and Neurosciences (NIMHANS), Bangalore, India.
Address for correspondence: Dr Dhanya Raveendranathan, Department of Psychiatry, National Institute of Mental Health And Neurosciences, Bangalore 560029, India.
Tel: (91-80) 26995250; Fax: (91-80) 26564822; Email: dhanya.ravi@gmail.com
An earlier version of this paper was presented at The Second Joint International Conference of the Hong Kong College of Psychiatrists and the Royal College of Psychiatrists (UK) — Brain, Behaviour and Mind 2010 (poster).
Submitted: 12 December 2011; Accepted: 26 January 2012
Abstract
Objective: Violence in psychiatric wards results in serious consequences and there is need for research to assess it in various settings to enable improvements in safety within psychiatric facilities. This study aimed to assess the inpatient violence from victims’ perspective, in settings where family members accompanied patients during inpatient stay and played a significant role in caregiving.
Methods: A total of 100 consecutive incidents of inpatient violence were examined. Family members present at the time of the incident were interviewed to assess putative causes and behaviour prior to the incident.
Results: Bipolar spectrum disorder was the most common diagnosis. Family members were the targets of violence in 70% of the incidents and 81% were provoked episodes. Also, 76% of the patients were identified by family member to be irritable just prior to the episode. As preventive measures, family members suggested a need for more staff, more sedation, and improved communication.
Conclusions: The capability of family members to identify behaviour patterns of patients prior to the episode might help decrease the severity and consequence of violence. It is essential to provide culture- specific interventions to the family, which could enable them in handling violence and give better care for the patient.
Key words: Family; Inpatients; Violence
摘要
目的:精神病房内的暴力行为可导致严重後果。因此,有关这种行为在各种护理环境的评估研究是需要的,以助改善精神病院的安全。本研究以家庭成员作为患者住院时的主要陪伴和照顾者的环境,从受害者角度分析後者的暴力行为。
方法:连续检视100宗住院患者的暴力行为,并与目睹事件发生的家庭成员面谈,从而了解他们对患者事发前行为的观察和推敲导致暴力行为的因素。
结果:最常见的诊断是躁鬱症。在70%暴力事件中,家庭成员是受害目标,而81%的暴力事件则由家庭成员引发出来的。此外,家庭成员能确定76%患者在暴力事件前有急燥情绪。家庭成员建议的预防措施包括增添医院职员、增加镇静剂份量和改善与患者之间的沟通。
结论:家庭成员如能辨识患者在暴力事件前的行为,便可减低事件的严重性和後果。为家庭成员提供文化特异干预方案也有助他们处理患者的暴力行为,且为患者提供更好的照顾。
关键词:家庭、住院病人、暴力行为
Introduction
In India, for more than 50 years, there was a practice of involving family members in the caretaking process for inpatients by asking them to stay with the patient during the period of hospitalisation. This practice is believed to enable faster recovery than patients admitted without accompanying family members.1 By custom, families assume the role of principal caregivers for their ill relatives because of strong family relationships resulting in mutual interdependence and concern for relatives during adversity. An earlier study from India assessing the role of caregivers in patients with chronic schizophrenia found that in the majority of cases, family members were responsible for looking after their relative during inpatient stay and at home.2 India has a huge population of subjects with psychiatric disorders and faces a severe shortage of mental health professionals.3 Hence, a system of utilising the services of the family members has multiple advantages. These include assisting the limited staff available so as to facilitate a greater degree of personalised and better care for patients.4 Thus, having adequate support from the family is of great benefit to the patient, the clinician, and health care administrators.
Violent patients in a psychiatric hospital pose a considerable challenge to psychiatric staff and health planners, because of the risks to the individuals involved and the implications for the organisation of services. These include longer hospitalisation, greater need for tranquilising medications, and more frequent medication changes, all of which have serious cost implications. Studies of inpatient violence are hard to compare because of differing definitions of violence and hospital settings in which the studies took place. A few western studies only focused on violence from the perspective of the staff and patients. It is important to recognise that the family members pay a huge price in the form of emotional, financial, psychological, and social burdens in the process of caring for relatives with psychiatric disorders, according to the western studies5-8 and those from India.9-11
Although there have been studies looking at the caregiver burden on family members in a variety of domains, there have been none from the perspective of family members as victims of violence in a psychiatric setting where they stay with the patients during inpatient care. Hence, this study set out to examine this issue in an Indian setting.
Methods
The study was conducted in the adult psychiatric wards of National Institute of Mental Health and Neurosciences, a tertiary care psychiatric teaching hospital of Bangalore in southern India. The study was approved by the institutional ethics committee. A total of 100 consecutive incidents involving male and female inpatients exhibiting violent behaviour during the period April 2008 to July 2009 were included. Violence was defined as the use of physical force the National Institute of Clinical Excellence guidelines.12 It includes physical violence (which required physical contact with victims) and non-physical violence (including difficulty reporting verbal aggression in crowded wards and the possibility of underreporting, it was excluded from the study unless concomitant threatening or physical aggression took place. The definition of violence used for the study also and to other objects. In other words, violent incidents committed only against other people were included. Sexual violence including inappropriate physical contact made by the patient against any other person was also not included as this was considered outside the purview of this study. Besides, repeated episodes of violence by the same patient were excluded. Diagnosis was made by 2 independent trained psychiatrists based on the ICD-10 criteria.13 Patients with an exclusive diagnosis of substance dependence in the absence of any other co-morbid psychiatric illness like induced psychosis were excluded. Information regarding violent incidents in the adult psychiatric wards occurring in the previous 24 hours was obtained from the staff nurse twice daily (in the morning and the evening). The clinical and socio-demographic details of the patients were collected partly using the information available in the patient treatment file and partly from interviews with a family member. The family member (who was present at the time of the incident) was interviewed within 24 hours of the incident, using the semi-structured interview schedule devised for this study after obtaining written informed consent. The semi-structured interview schedule contained open-ended questions to gather information regarding the behaviour of the patient prior to the incident, perceived causes, and suggestions regarding further preventive measures from family members. The semi-structured interview schedule contained the following questions — “How was the patient behaving a day prior / 2 hours prior / immediately prior to the incident?”, “What do you think are the possible causes that led to the incident?”, “How satisfied are you with the way it was managed?”, “What help was available?”, “What help was required?”, “How much time did it take for adequate help to arrive?”, and “Any possible ways to prevent this incident from recurring or minimising the damage?”
The responses were recorded verbatim after face-to- face interviews with the respondents. All interviews were conducted by the principal investigator (the first author).
Results
Table 1 shows the socio-demographic and clinical profile of the patients who were responsible for the 100 episodes of violence.
The mean (standard deviation) age of the study sample was 29 (11) years. Their psychiatric diagnoses were divided into 3 major groups: affective disorder, non- affective psychotic disorder, and other diagnosis. Non- affective psychotic disorder included various subtypes of schizophrenia, psychosis not otherwise specified, acute psychosis, and substance-induced psychosis. Affective disorder included the first episode of mania and bipolar affective disorder. Other diagnoses included personality disorders, obsessive compulsive disorders, organic conditions, and mental retardation. Bipolar spectrum disorders were noted in 52 patients, while the schizophrenia spectrum was present in 25 and other diagnoses in 23 patients. Bipolar affective disorder, with a current episode of mania with psychotic symptoms (31 cases), was the most common diagnosis.
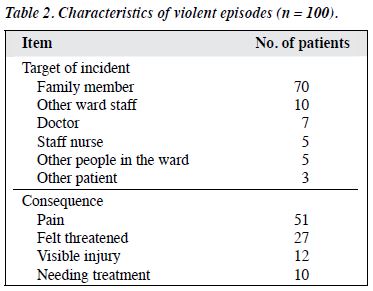
For 78% of the patients, there was a history of violence in the previous month. About 70% of incidents were preceded by a clear threat made by the patient, which comprised verbal threats (72%) and physical threats (28%). The characteristics of the violent incidents are described in Table 2.
In 70%, a family member was the target of the violence. In 81 incidents, a clear provocation for the violence was identified. In this study, provocation was defined as clearly identifiable external provocation by the victims. In 63 (78%) of the incidents, the provocation was identified 7 by the patient’s family member. Of the 75 (38 male and 5 37 female) family members of patients interviewed, 54 5 were parents, 13 were siblings, 6 were spouses, and 2 were 3 children. All the questions in the interview schedule were to each question varied. The behaviour of the patient at 51 time points 1 day, 2 hours, and just before the incident 27 were obtained from the family member as shown in Table 3.
One day prior to the incident, 50 (67%) were identified 10 as irritable by the family member. Two hours prior to the incident, 57 (76%) of the family members identified the patients as being irritable. The causes of the violent incident as perceived by the family member are shown in Table 3; of which the patient being prevented from leaving the hospital ward (57%) was the commonest reason.
The recommendations made by family members regarding the means to prevent similar incidents could be divided into 3 themes (Table 4).
Numerous recommendations were made on changes in hospital administration and policy, including issues related to staffing and restricting patient access to sharp objects (glass and knives) that could be used as weapons. The most common recommendation (52%) was to retain more staff on duty in the ward in the form of nurses and security personnel. There were a few treatment recommendations, such as frequent administration of sedating medication (19%) and recourse to isolation wards (4%). There were also a few recommendations to improve communication with patients, including the need to listen carefully to their initial pleas and respond appropriately without an outright immediate refusal. In all, 12 (16%) family members offered no recommendations.
Discussion
A family member is an untrained individual who, as per the hospital policy, accompanies the patient during a hospital stay and has the closest contact with him or her. In this study, the most common victim of violence was the family member. Violent episodes were noted in patients with a wide variety of disorders. A majority had a history of violence in the previous month and most incidents were preceded by a clear threat made by the patient. There is a consensus that a history of aggressive behaviour is the best predictor of future violence.14-19 These findings underscore the need to carefully monitor patients who have a history of violence.
Among the 81 provoked episodes, more than 75% were by a family member. The causes included their patient being prevented from leaving the ward, getting upset over the family member who reported to staff about their violent behaviour, and strict ward rules enforced by the staff. These were in fact highly modifiable causes for violence and could have been prevented by negotiating with the patient by practising a form of pre-incident verbal de-escalation. The staff’s perspective of possible causes for violence was comparable to that perceived by the family members, except that the former identified the patient’s disoriented state as a cause (in about 5% of instances). This finding was consistent with several studies20-22 showing that external provocations, involving problematic interpersonal interactions, are the most common situations leading to inpatient violence. In the majority of incidents, the family members could identify specific patient behaviour patterns prior to the violent incident, which could be used as warning signals and might have helped involved individuals identify the impending incident. Lee et al23 concluded that behaviour patterns of patients immediately before incidents might have better predictive value than the diagnosis per se. Since violence is unpredictable in many situations, rather than preventing it, these behaviour patterns could help in taking precautionary measures so as to decrease the severity and consequences of violent incidents.
Family members made several recommendations to prevent future episodes of violence. They included administrative steps (increased staffing and treatment changes) and the increased use of sedative medications. The latter was often perceived as the most practical form of prevention to mitigate inpatient violence due to its rapid onset of action. Chemical restraint is usually achieved by resorting to parenteral antipsychotic medication and / or benzodiazepines. Frequent use of many of these medications increases the risk of extrapyramidal side-effects like acute dystonia. Family members should be made aware of these side-effects and the importance of alerting staff on duty at the earliest manifestation of such features.
Three large-scale international collaborative studies conducted by the World Health Organization — the International Pilot Study on Schizophrenia,24 the Determinants of Outcome of Severe Mental Disorders,25 and the International Study of Schizophrenia26 — convincingly demonstrated that persons with schizophrenia had a better clinical outcome in India and other developing countries, compared with their western counterparts and that much of this was attributed to good family support in these countries. Family members in India assume a multitude of roles in the caregiving of patients as shown by an earlier study from our centre.2 Such care ranged from accompanying the patient during inpatient stays to ensuring medication adherence. Hence, the role of family members in the care of patients in a country like India cannot be ignored due to important cultural and logistic reasons.
Several studies conducted in India27-29 demonstrated the importance of culture-specific and flexible psycho- educational programmes, which included identifying relapse symptoms and treatment-related information. This may also improve patient compliance, resulting in better illness outcomes and caregiver satisfaction. In a country facing significant shortage of mental health professionals, the capability of family members in identifying behaviour patterns of the patient prior to the episode could help to prevent or ease the management of such incidents.
It is necessary to identify the distress of family members while they face inpatient violence. Including this aspect of patient care as part of the psycho-education for family members makes it more culture-specific and provides them with the skills in handling such patients during their admissions and post-discharge. It may also go a long way towards relieving an important aspect of the caregiver burden in managing a psychiatrically ill relative because even after they are discharged from the hospital, their family members continue to remain the main source of patient care in the community. Ultimately, prevention of a violent incident ensures the safety of both the victim and the patient.
One of the limitations of this study was its relatively small sample size. As the study was undertaken in a hospital, its generalisability to other settings like the community is limited. In the absence of a control group, definitive predictors of inpatient violence could not be made. Lack of a structured evaluation for clinical factors like severity of psychotic symptoms and premorbid personality is also acknowledged. Nevertheless, this study highlights a very important, though poorly examined aspect of psychiatric practice and care.
References
- Avasthi A. Preserve and strengthen family to promote mental health. Indian J Psychiatry 2010;52:113-26.
- Samuel M, Thyloth M. Caregivers’ roles in India. Psychiatr Serv 2002;53:346-7.
- Kharawala S, Dalal J. Challenges in conducting psychiatry studies in India. Perspect Clin Res 2011;2:8-12.
- Kohlmeyer WA, Fernandes X. Psychiatry in India: family approach in the treatment of mental disorders. Am J Psychiatry 1963;119:1033-7.
- Fadden G, Bebbington P, Kuipers L. The burden of care: the impact of functional psychiatric illness on the patient’s family. Br J Psychiatry 1987;150:285-92.
- Onwumere J, Kuipers E, Bebbington P, Dunn G, Fowler D, Freeman D, et al. Caregiving and illness beliefs in the course of psychotic illness. Can J Psychiatry 2008;53:460-8.
- Scazufca M, Kuipers E. Coping strategies in relatives of people with schizophrenia before and after psychiatric admission. Br J Psychiatry 1999;174:154-8.
- Budd RJ, Oles G, Hughes IC. The relationship between coping style and burden in the carers of relatives with schizophrenia. Acta Psychiatr Scand 1998;98:304-9.
- Chakrabarti S, Kulhara P. Family burden of caring for people with mental illness. Br J Psychiatry 1999;174:463.
- Chakrabarti S, Raj L, Kulhara P, Avasthi A, Verma SK. Comparison of the extent and pattern of family burden in affective disorders and schizophrenia. Indian J Psychiatry 1995;37:105-12.
- Kalra H, Nischal A, Trivedi JK, Dalal PK, Sinha PK. Extent and determinants of burden of care in Indian families: a comparison between obsessive-compulsive disorder and schizophrenia. Int J Soc Psychiatry 2009;55:28-38.
- Wright S, Gray R, Parkes J, Gournay K. The recognition, prevention and therapeutic management of violence in acute in-patient psychiatry. A literature review and evidence-based recommendations for good practice. United Kingdom Central Council for Nursing, Midwifery and Health Visiting; 2002.
- The ICD-10 Classification of Mental and Behavioural Disorders. Geneva: World Health Organization; 1992.
- Noble P, Rodger S. Violence by psychiatric in-patients. Br J Psychiatry 1989;155:384-90.
- Shah AK, Fineberg NA, James DV. Violence among psychiatric inpatients. Acta Psychiatr Scand 1991;84:305-9.
- Davis S. Violence by psychiatric inpatients: a review. Hosp Community Psychiatry 1991;42:585-90.
- El-badri SM, Mellsop G. Aggressive behaviour in an acute general adult psychiatric unit. Psychiatrist 2006;30:166-8.
- Owen C, Tarantello C, Jones M, Tennant C. Violence and aggression in psychiatric units. Psychiatr Serv 1998;49:1452-7.
- Grassi L, Peron L, Marangoni C, Zanchi P, Vanni A. Characteristics of violent behaviour in acute psychiatric in-patients: a 5-year Italian study. Acta Psychiatr Scand 2001;104:273-9.
- Powell G, Caan W, Crowe M. What events precede violent incidents in psychiatric hospitals? Br J Psychiatry 1994;165:107-12.
- Palmstierna T, Huitfeldt B, Wistedt B. The relationship of crowding and aggressive behavior on a psychiatric intensive care unit. Hosp Community Psychiatry 1991;42:1237-40.
- Quanbeck CD, McDermott BE, Lam J, Eisenstark H, Sokolov G, Scott CL. Categorization of aggressive acts committed by chronically assaultive state hospital patients. Psychiatr Serv 2007;58:521-8.
- Lee HK, Villar O, Juthani N, Bluestone H. Characteristics and behavior of patients involved in psychiatric ward incidents. Psychiatr Serv 1989;40:1295-7.
- Report of the international pilot study of schizophrenia. Volume 1. Geneva: World Health Organization; 1973.
- Jablensky A, Sartorius N, Ernberg G, Anker M, Korten A, Cooper JE, et al. Schizophrenia: manifestations, incidence and course in different cultures. A World Health Organization ten-country study. Psychol Med Monogr Suppl 1992;20:1-97.
- Mason P, Harrison G, Glazebrook C, Medley I, Croudace T. The course of schizophrenia over 13 years. A report from the International Study on Schizophrenia (ISoS) coordinated by the World Health Organization. Br J Psychiatry 1996;169:580-6.
- Ismail Shihabuddeen TM, Gopinath PS. Group meetings of caretakers of patients with schizophrenia and bipolar mood disorders. Indian J Psychiatry 2005;47:153-6.
- Thara R, Padmavati R, Lakshmi A, Karpagavalli P. Family education in schizophrenia: a comparison of two approaches. Indian J Psychiatry 2005;47:218-21.
- Kulhara P, Chakrabarti S, Avasthi A, Sharma A, Sharma S. Psychoeducational intervention for caregivers of Indian patients with schizophrenia: a randomised-controlled trial. Acta Psychiatr Scand 2009;119:472-83.