East Asian Arch Psychiatry 2012;22:57-61
ORIGINAL ARTICLE
Factors related to Choosing Psychiatry as a Future Medical Career among Medical Students at the Faculty of Medicine of the University of Indonesia
印尼大学医科生选择从事精神医学的因素
Dr Tjhin Wiguna, MD, MIntMH, PhD, Child and Adolescent Psychiatry Division, Department of Psychiatry, University of Indonesia, Jakarta, Indonesia. Dr Kai-Sing Yap, University of Indonesia, Jakarta, Indonesia.
Dr Boey-Warn Tan , University of Indonesia, Jakarta, Indonesia. Dr Terence Siew, University of Indonesia, Jakarta, Indonesia.
Dr John Danaway, University of Indonesia, Jakarta, Indonesia.
Address for correspondence: Dr Tjhin Wiguna, Child and Adolescent Psychiatry Division, Department of Psychiatry, University of Indonesia, Jl. Salemba Raya 4, Jakarta 10430, Indonesia.
Tel: (62-21) 3107741; Fax: (62-21) 39899128; Email: twiga00@yahoo.com
Submitted: 26 August 2011; Accepted: 26 January 2012
Abstract
Objective: To identify factors related to choosing psychiatry as a future medical career and attitude towards psychiatry among medical students of the International Class Programme of the Faculty of Medicine, The University of Indonesia.
Methods: This was a cross-sectional design which included 225 data sets from first to sixth year medical students (n = 188) as well as the freshly graduated medical doctors (n = 37). The Attitude Towards Psychiatry–30 questionnaire (ATP-30) was adopted. Data including demographics, past experience in psychiatry, inclination to work in psychiatry, and 3 specialty choices for future medical career were collected. Independent t test and logistic regression were used in data analysis.
Results: The mean ATP-30 score from the fresh graduates was slightly higher compared with the medical students. Inclination to work in the field of psychiatry, past experience in psychiatry, and the ATP-30 score were significantly correlated and contributed 57% to the prediction of choosing psychiatry as a future medical career (p < 0.05).
Conclusion: The greater inclination to work in the field of psychiatry, as well as a better attitude towards psychiatry can predict the choice of psychiatry as a future medical career. Therefore, it is very important to increase the quality of psychiatry teaching and to motivate medical students who show a high level of interest in psychiatry.
Key words: Career choice; Questionnaires; Students, medical
摘要
目的:检视印尼医科大学国际班医科生选择从事精神医学的因素和态度。
方法:这项横断面研究纳入225名1年级至6年级医科生(n = 188)和应届毕业医科生(n = 37)的数据,并采用30项精神医学态度(ATP-30)问卷。研究也收集其他数据如人口统计学、与精神医学相关的个人经验、从事精神医学的倾向性,以及首3个专科就业意愿。研究也使用独立样本t 检定和逻辑迴归分析作数据分析。
结果:应届毕业医科生的平均ATP-30比分较其他医科生略高。倾向从事精神医学、与精神医学相关的个人经验,以及ATP-30比分与选择从事精神医学呈显著相关,并占预测因素的57%(p < 0.05)。
结论:倾向从事精神医学和对这科的态度为选择从事精神医学的预测因素。因此,改善精神医学教学质素,以及激发对精神医学兴趣浓厚的医科生的学习潜能是非常重要的。
关键词:职业选择、问卷、学生,医科
Introduction
The Faculty of Medicine of The University of Indonesia (FMUI) announced the International Class Programme in 2000, using English as the basic medium of instruction. It aims to train up medical doctors who can compete with those from other countries and possess internationally recognised competencies.
The system of teaching and learning is mostly student-based and problem-based. From the first to the sixth semester the curriculum consists of medical science education, integrated basic medical science, and basic clinical skills. Students are exposed to neuropsychiatry in the Neuroscience module, psychosocial development in the Growth and Development module, and finally they go to the Neurology and Psychiatry module for 6 weeks. During that period, students do not have any exposure to patients.
After finishing the third year, they are sent to the University of Melbourne, Australia for research activities for a year. During the fifth and sixth years, they are posted to undertake clinical practice in several departments. Clinical practice in the Department of Psychiatry is run over a 3-week period. They work with inpatient and outpatient clinics and finally have to record their case and present it at an oral examination.
Research on the attitude of medical students towards psychiatry was extensively documented many years ago. The aim of this research was to determine what difficulties there were in recruiting medical graduates to specialise in psychiatry.1,2 The study from Al-Ansari and Alsadadi3 showed that the first, fourth, and seventh year medical students’ exposure to psychiatry did not improve their Attitude Towards Psychiatry–30 (ATP-30) score. In addition, few reports demonstrated any positive attitudinal change towards psychiatry among medical students following exposure to the psychiatry teaching programme.4,5
Several studies showed that the number of people with mental disorders has been increasing worldwide, nevertheless only a small proportion of medical graduates were willing to pursue this specialty.6,7 Notably, the number of international medical graduates with the intention of choosing psychiatry as their future medical specialty decreased from approximately 10% in the 1960s, to only about 2 to 5% in the last decade.8-11 A study in Ireland6 also reported that only 4% of interns considered psychiatry as a career choice. Maric et al12 also reported that medical students at the School of Medicine, University of Belgrade, Serbia viewed psychiatry as a much less attractive clinical specialty compared with internal medicine, surgery, paediatrics, as well as obstetrics and gynaecology.
We understand that medical students from the FMUI are potential psychiatry residents for our department. However, from the 5 batches of medical students (190 in all) graduated from the International Class Programme to date, only 1 applied for the post of the resident at the Department of Psychiatry, The University of Indonesia.
There have been several studies to identify factors associated with the declining interest in psychiatry that have resulted in several hypotheses to explain this phenomenon, one of which is related to the attitude of medical students towards psychiatry.13-16 Therefore, it is important to identify such attitudes and other related factors, in order to address reasons for their lack of interest.
Methods
This was a cross-sectional study using secondary data collected from medical students of the International Class Programme of the FMUI, when they were posted in the Research module (March to May 2011). To answer our research questions, we categorised the subjects into 3 groups, namely first to third year students who had already received basic psychiatry teaching but had not completed the clinical rotation in psychiatry (group 1); fifth and sixth year students who had finished their clinical rotation in psychiatry (group 2); and first and second year graduate students (doctors) [group 3].
There were 276 medical students and 96 doctors (freshly graduated medical students in 2011) eligible for this study, but only 225 fulfilled the inclusion criteria of completing the entire questionnaire. They comprised 96 subjects from group 1, 92 from group 2, and 37 from group 3.
The original version of the ATP-30 developed by Burra et al4 was adopted, as the students in this study came from several countries that English was the medium of instruction. It consists of 30 statements expressing the extent of agreement or disagreement towards mental illnesses, psychiatric patients, psychiatric institutions and psychiatrists, teaching, knowledge and career choice, using a 5-point Likert scale (1 = strongly agree, 2 = agree, 3 = neutral, 4 = disagree, 5 = strongly disagree). The total score ranged from 30 to 150. The higher the score, the more favourable the attitude towards psychiatry. Other data consisting of age, gender, top 3 medical specialty choices, inclination to work in the field of psychiatry as a future career, as well as their past experience in psychiatry were also recorded. Inclination to work in the field of psychiatry was rated on a scale from 0 (no inclination) to 9 (extreme inclination).
Data were analysed using the SPSS Windows version 16.0. The Kolmogorov-Smirnov test was used to analyse for normality of distributions. The one-way analysis of variance and t test were used to compare the ATP-30 scores among the groups. Logistic regression analysis was also performed to quantify factors related to choosing psychiatry as their future medical specialty. A p value of < 0.05 was considered statistically significant in our study.
Results
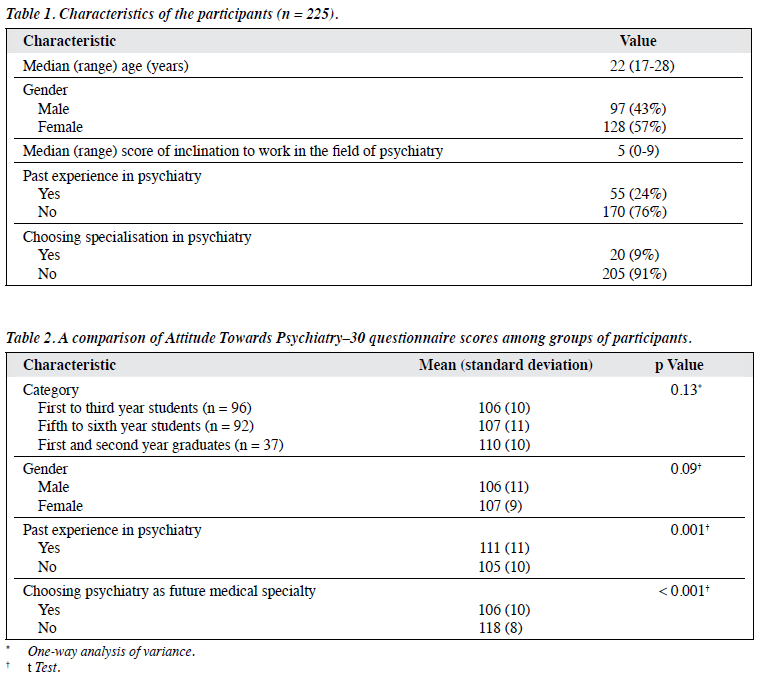
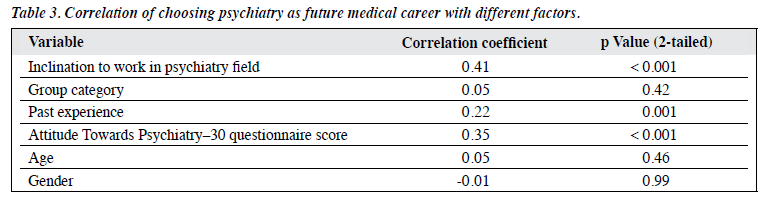
The age of the participants ranged from 17 to 28 years (Table 1). The male-to-female ratio was approximately 1:1.3. Overall, the participants had a good attitude towards psychiatry with a mean (standard deviation) ATP-30 score of 107 (10). The fresh graduates had the highest mean ATP-30 score compared with the other 2 groups (Table 2). No significant differences in mean ATP-30 scores among these 3 groups (p = 0.13) as well as that between male and female participants (p = 0.09) were found.
About 25% of the medical students had past experience in psychiatry, for example, some had family members (parents, brothers or sisters) with depression, anxiety or psychotic disorders. Thus, they had had contact with psychiatrists, whilst others had friends or relatives with mental health problems such as adjustment problems in the workplace or while attending school. Their inclination score to work in the field of psychiatry ranged from 0 to 9, with a median of 5.
The medical students were asked to rank the 3 most preferred medical specialties after finishing medical school. Internal medicine, paediatrics, and cardiology were the 3 highest-ranked choices. The proportion of medical students choosing psychiatry as one of their preferences was 9%, and was ranked in twelfth by popularity.
There was a statistically significant moderate correlation between choosing psychiatry as a future medical specialty and ATP-30 score, past experience in psychiatry, and an inclination to work in the field of psychiatry. Interestingly, there was no correlation of choosing psychiatry as a future medical specialty with gender, age, and group category.
Logistic regression analysis showed that inclination to work in psychiatry field, past experience in psychiatry, as well as mean ATP-30 score were significantly correlated with choosing psychiatry as future medical career (Table 3). Among these, inclination to work in psychiatry field contributed higher for choosing psychiatry as future medical career compared with the other 2 variables. These 3 variables contributed 57% to the prediction of choosing psychiatry as future medical career (p < 0.05).
Discussion
Our findings showed that attitude towards psychiatry changed positively in line with the higher medical education, although such changes were not statistically significant. However, we observed differences in the mean ATP-30 scores between the 3 groups; the first to third year medical students had the lowest mean ATP-30 score. This finding might be attributable to the very gradual exposure to psychiatry in the teaching curriculum; at the beginning there was an emphasis on neurosciences, empathy, growth and development, and only in the fifth semester were the medical students introduced to neurology and psychiatry (in a 6-week module). During the first 3 years, the students had mostly been exposed only to historical case studies (to trigger group discussion) and had not yet encountered patients.
The clinical rotation in specialties was in small groups and run as 3-week courses in each department (except for Paediatrics, Internal Medicine, Obstetrics and Gynaecology, and Surgery). The psychiatry clinical rotation consisted of several methods of teaching, namely topic discussions related to mental disorders and mental health issues, psychiatric interviews and mental state examinations for inpatients and outpatients, psycho-education for patients and their families, and home visits.
From the beginning of psychiatric teaching, we strongly emphasised both the bio-psychosocial approach and the multi-axial diagnosis. Students were usually asked to identify the psychosocial aspects of each patient, not only for patients in the psychiatry ward or outpatient clinic but also for other patients in general. This style of teaching and the empathy module played an important role in broadening the medical students’ frame of view in looking at the patients. By this means they were expected to regard the patient holistically rather than focus only on the specific illness.
After graduating from the medical school, the graduates were expected to apply this approach in their daily practice. It was assumed that every time they met patients, they would try to understand them more and automatically remember what they had learnt in the psychiatry and empathy module. This may explain why the freshly graduated medical students had a higher mean score on ATP-30 scale. In general, it could be inferred that the whole process in the International Class Programme curriculum at the FMUI contributed significantly to positive attitudes towards psychiatry among these fresh graduates.
In line with worldwide studies which showed that psychiatry is less popular than other medical specialties, our study also revealed such findings in that psychiatry was not included in the top 10 medical specialties for a future career. The proportion of medical students who were willing to pursue psychiatry as their future specialty was slightly higher (9%) than that reported in Ireland (4%),6 Australia (1%),7 and the United Kingdom (0.5%).17
In our study, several factors correlated with choosing psychiatry as a future medical career, but inclination to work in the psychiatry field yielded a higher correlation than the others. Surprisingly, choosing psychiatry as future medical career did not correlate with age, gender, and our study groups. It can be assumed that inclination is a subjective feeling; it is believed that a person who is so inclined is more motivated to learn more, elaborate deeper, and show a better attitude. A study by McParland et al18 revealed that ATP-30 score increased positively following the intention to participate in the psychiatry specialty. Moreover, it appeared that those who ruled out psychiatry as their future medical specialty perceived it as lacking a scientific foundation and clinical efficacy in the context of treatment, and also feared emotional drainage from interacting with psychiatric patients.
In our study, medical students who chose psychiatry as their future medical career had more inclination to work in that field and also had a better attitude towards the specialty, whereas past experience in psychiatry did not play a significant role. Conceivably, past experience in psychiatry might add positive as well as negative impacts about the discipline. A previous study by Balon et al19 showed that medical students had various perspectives on psychiatry, including having low prestige compared with other medical specialties, being unscientific and imprecise compared with other rapidly expanding frontiers of medicine. This study19 also revealed that medical students viewed psychiatrists as clear and logical thinkers, too apologetic when teaching the subject, being odd, abusing their legal power to hospitalise patients against their will, and playing a good role model in the psychiatry clinical rotation. In the same study,19 the medical students mentioned that although they were interested in psychiatry, their medical school made no effort to encourage their willingness to become a psychiatrist.
A study by Zimny and Sata20 concluded that psychology-based college courses and mental health working experience influenced choosing psychiatry as a future medical specialty, but our study did not examine these variables. Furthermore, it is understood that when a medical student chose psychiatry as a future career, he / she would be more inclined to work in that field and have better perspectives and attitude towards the subject. By this means they could show their responsibility and professionalism to other medical professionals, patients, and family members.
The results of this study might provide future directions for psychiatry teaching in the FMUI International Class Programme. These could target introducing and improving evidence-based teaching, especially in relation to neuroscience and neurodevelopment, and in turn provide more depth and background for the appreciation of psychiatric disorders. Being a good role model in psychiatry clinical work is a must for psychiatrist, so as to reduce the associated stigma, especially among other medical professionals. This could induce a positive atmosphere in the teaching environment. It could also encourage medical students to pursue the area as their future medical specialty by giving clear examples for an imminent career in psychiatry, especially if the student already shows an inclination. Longer periods of clinical clerkship could be introduced to afford ample time for students to comprehend the essence of being a psychiatrist and remove the associated stigma. It is vital to nurture interests from the early years of medical school. These measures are important because medical students of today are the pillars of the medical force tomorrow. Without committed recruitment into the psychiatric field, the dwindling supply of psychiatrists will not meet the rising demand. Our subjects were the medical students from the FMUI International Class Programme, therefore our findings should be interpreted cautiously in other settings as they may not be representative of medical students from other universities in Indonesia.
References
- Lambert TW, Goldacre MJ, Turner G. Career choices of United Kingdom medical graduates of 1999 and 2000: questionnaire surveys. BMJ 2003;326:194-5.
- Sierles FS, Taylor MA. Declines of U.S. medical student career choice of psychiatry and what to do about it. Am J Psychiatry 1995;152:1416- 26.
- Al-Ansari A, Alsadadi A. Attitude of Arabian Gulf University medical students towards psychiatry. Educ Health (Abingdon) 2002;15:180-8.
- Burra P, Kalin R, Leichner P, Waldron JJ, Handforth JR, Jarrett FJ, et al. The ATP 30 — a scale for measuring medical students’ attitudes to psychiatry. Med Educ 1982;16:31-8.
- Glynn S, Reilly M, Avalos G, Mannion L, Carney PA. Attitudinal change toward psychiatry during undergraduate medical training in Ireland. J Psych Med 2006;23:131-3.
- Finucane P, O’Dowd T. The career plans of Irish interns: results of a national survey. Ir Med J 2004;97:149.
- Malhi GS, Parker GB, Parker K, Kirkby KC, Boyce P, Yellowlees P, et al. Shrinking away from psychiatry? A survey of Australian medical students’ interest in psychiatry. Aust N Z J Psychiatry 2002;36:416-23.
- Malhi GS, Parker GB, Parker K, Carr VJ, Kirkby KC, Yellowlees P, et al. Attitudes toward psychiatry among students entering medical school. Acta Psychiatr Scand 2003;107:424-9.
- Kuhnigk O, Strebel B, Schilauske J, Jueptner M. Attitudes of medical students towards psychiatry: effects of training, courses in psychiatry, psychiatric experience and gender. Adv Health Sci Educ Theory Pract 2007;12:87-101.
- Ghadirian AM, Engelsmann F. Medical students’ attitude towards psychiatry: a ten-year comparison. Med Educ 1982;16:39-43.
- 1 Baboolal NS, Hutchinson GA. Factors affecting future choice of specialty among first-year medical students of the University of the West Indies, Trinidad. Med Educ 2007;41:50-6.
- Maric NP, Stojiljkovic D, Milekic B, Milanov M, Bijelic J. Change of students interest in psychiatry over the years at school of medicine, University of Belgrade, Serbia. Isr J Psychiatry Relat Sci 2011;48:42-8.
- Ndetei DM, Khasakhala L, Ongecha-Owuor F, Kuria M, Mutiso V, Syanda J, et al. Attitudes toward psychiatry: a survey of medical students at the University of Nairobi, Kenya. Acad Psychiatry 2008;32:154-9.
- Baptista T, Pérez CS, Méndez L, Esqueda L. The attitudes toward psychiatry of physicians and medical students in Venezuela. Acta Psychiatr Scand 1993;88:53-9.
- Wilkinson DG, Greer S, Toone BK. Medical students’ attitudes to psychiatry. Psychol Med 1983;13:185-92.
- Pan PC, Lee PW, Lieh-Mak FF. Psychiatry as compared to other career choices: a survey of medical students in Hong Kong. Med Educ 1990;24:251-7.
- Goldacre MJ, Turner G, Fazel S, Lambert T. Career choices for psychiatry: national surveys of graduates of 1974-2000 from UK medical schools. Br J Psychiatry 2005;186:158-64.
- McParland M, Noble LM, Livingston G, McManus C. The effect of a psychiatric attachment on students’ attitudes to and intention to pursue psychiatry as a career. Med Educ 2003;37:447-54.
- Balon R, Franchini GR, Freeman PS, Hassenfeld IN, Keshavan MS, Yoder E. Medical students’ attitudes and views of psychiatry: 15 years later. Acad Psychiatry 1999;23:30-6.
- Zimny GH, Sata LS. Influence of factors before and during medical school on choice of psychiatry as a specialty. Am J Psychiatry 1986;143:77-80.