Hong Kong J Psychiatry 2007;17:3-9
ORIGINAL ARTICLE
Attitudes of Healthcare Professionals towards Psychiatric Patients in a General Hospital in Hong Kong
香港一所普通科醫院的醫護人員對精神病患者的態度
LY Chow, WK Kam, CM Leung
周禮賢, 金偉幗, 梁志明
Dr LY Chow, MBChB, MRCPsych, Grad. Dip. Child P.S. (Monash), FHKCPsych, FHKAM (Psychiatry), Department of Psychiatry, Shatin Hospital, Hong Kong, China.
Dr WK Kam, MBChB, MRCPsych, FHKCPsych, FHKAM (Psychiatry), Department of Psychiatry, Tai Po Hospital, Hong Kong, China.
Dr CM Leung, MBBS, MRCPsych, FHKCPsych, FHKAM (Psychiatry), Department of Psychiatry, Shatin Hospital, Hong Kong, China.
Addresses for correspondence: Dr LY Chow, Department of Psychiatry, Shatin Hospital, 33 A Kung Kok Street, Ma On Shan, Hong Kong, China.
Tel: (852) 2636 7748; Fax: (852) 2647 5321; E-mail: laiyinchow@hotmail.com
Submitted: 23 January 2007; Accepted: 13 March 2007
Abstract
Objectives: To examine the attitudes of healthcare professionals towards psychiatric patients in a general hospital in Hong Kong, and explore what contributions these attitudes may have on their management.
Participants and Methods: A survey was carried out on healthcare professionals working in a general hospital in Hong Kong. A newly devised questionnaire with a case vignette was used. Each subject received a case depicting either a psychiatric patient (case group) or a diabetes mellitus patient (control group) randomly.
Results: A total of 1200 questionnaires were distributed with a response rate of 36.1%. A case vignette depicting a psychiatric patient elicited responses that reveal a statistical significant contribution towards the expression of negative opinions; about two-thirds of the statements contained negative connotations. Increase in social exposure to psychiatric patients led to a decrease in negative attitude, whilst negative experience with psychiatric patients led to an increase in negative attitude.
Conclusion: Stigma towards psychiatric patients exists to a certain degree among the healthcare professionals in the general hospital we investigated. More clinical research is needed in this area to have a more in-depth understanding of the issue.
Key words: Attitude of health personnal; Mental disorders; Mentally ill persons; Stereotyping
摘要
目的:探討本港一所普通科醫院醫護人員對精神病患者所持的態度, 及其對治療病人的影響。
參與者與方法:研究以附帶病例的問卷方式進行。每位參與者隨機回答有關一名精病患者(研究組)或糖尿病患者( 對照組)的問題。
結果:共發出1200份問卷, 回應率為36. 1 % 。研究發現當問卷上所形容的為精神病患者時, 被訪者顯著地表達負面的意見; 約三份之二的受訪問題都是獲得負面的答案。增加醫護人員與精神病患者的社交接觸, 有助改善他們對精神病患者的態度; 但同時他們因照顧精神病患者所獲得的負面經驗越多,對病者的態度便越負面。
結論:在普通科醫院工作的醫讓人員, 對精神病患者抱有一定程度的負面態度, 須進行更多的臨床研究以作更深入的探討。
關鍵詞:醫護人員之態度、精神病、精神病患者、成見
Introduction
Mental health is recognised to be a major global health issue in the past century. The associated stigma is a distressing problem for persons suffering from mental illness and could have deleterious effects on all aspects of life.1-3 It lowered their self-esteem and affected their ability to socialise.4 On the other hand, attitudes of healthcare professionals may also affect the physical care psychiatric patients receive. People with mental illnesses were found to receive fewer medical services than the others.5 With a psychiatric history, family physicians were less likely to take physical complaints seriously.6 It was also noted that people who had been served by the mental health services had a mean of 8.8 years shorter life expectancy than controls.7 In another study, it was found that the presence of a substance use disorder significantly reduced the likelihood of beta-blocker use after myocardial infarction.8 Furthermore, people with mental illnesses had also had their chance of organ transplantation negated, merely on the grounds of their mental illnesses.9 Stigma could be a contributing factor underlying these various observations. The presence of stigma among healthcare professionals may impede the care-seeking of psychiatric patients.10
Different methodologies have been employed to ascertain attitudes towards people with mental illness. A literature review of 123 empirical articles11 found that nearly two-thirds were non-experimental surveys. Through the years, different standards for scales to study attitude have been devised.12-15 None was designed specifically to measure the attitude of healthcare professionals towards psychiatric patients. In general, previous studies revealed that negative attitudes towards psychiatric patients exist in the community. Among the various contributions explored, knowledge of mental illness and personal contact with psychiatric patients were the most widely investigated.16-18 Evidence related to the contribution of personal contact with psychiatric patients was conflicting. Increasing personal contact with psychiatric patients was found to either increase or decrease the negative attitude.19-21 In Hong Kong, increasing contact with psychiatric patients evidently decreased negative attitudes. Older persons and those with a lower education levels held more negative attitudes.22,23
Regarding healthcare professionals, junior nurses and those in training tended to be more pessimistic about the extent to which psychiatric patients were able to participate in treatment.24 Healthcare professionals were generally more pessimistic about the long-term outcomes of psychiatric patients than the general public.25,26 In a psychiatric hospital in Beijing, doctors were less authoritarian and restrictive than psychiatric nurses.27 Another study found that the medical students and doctors in a London teaching hospital held relatively less negative views towards psychiatric patients than the general public.28 The healthcare professionals expressed fear of not being able to predict how the patient would respond or behave; lack of knowledge being one of the major reasons.29 Studies done in Hong Kong were mainly focused on the general population, students, and mental health consumers.30,31 Hitherto, no local study has explored the attitudes of healthcare professionals towards psychiatric patients.
Patients and Methods
This study was part of a collaborative project to investigate stigma towards psychiatric patients among the healthcare professionals in 5 parts of Asia including Malaysia, South Korea, Thailand, The Philippines, and Hong Kong. A group of 8 experienced psychiatrists devised the questionnaire in 2004.
Questionnaire
The questionnaire had 3 parts. The first consisted of general questions on the demographics of the subjects, years of work experience, duration of psychiatric training, and work experience in psychiatric wards. In an open-ended question, the subjects were also asked to give 3 adjectives or phrases to describe how they perceived psychiatric patients. The second part consisted of 16 questions aiming to gauge the subject’s social exposure, work exposure, and negative experiences regarding psychiatric patients. They were also asked whether they had family members or friends who had suffered from mental illness. The third part of the questionnaire consisted of a case vignette with 19 statements. Opinions were measured on a 5-point Likert scale, ranging from ‘strongly disagree’, ‘disagree’, ‘neither disagree nor agree’, ‘agree’, to ‘strongly agree’. There were 2 versions of the case vignettes. The case set was a vignette describing a 24-year-old man (Mr X) who had psychiatric symptoms and needed to receive regular treatment from a psychiatric clinic. He was admitted to the subject’s ward for management of headache. The control vignette described another 24-year-old man (Mr Y), who suffered from poorly controlled diabetes mellitus, and was also admitted to the subject’s ward for management of headache. The 19 statements following the vignettes were the same for both case and control vignettes. They were common scenarios healthcare professionals working in a general ward setting would encounter during routine clinical practice.
Logistics of Opinion Survey
The original questionnaire was prepared in English, translated into Chinese and then back-translated. A pilot study was conducted in January 2005. The actual survey was carried out from February to April 2005 in the Prince of Wales Hospital of Hong Kong (a university teaching hospital and also a regional acute general hospital with 1315 beds). All nurses, interns, and doctors working in different clinical specialties in the hospital were potential subjects.
Questionnaires were distributed by 2 means. First, ward managers distributed questionnaires to individual nurses, who were asked to return them anonymously using an attached internal mail envelope or putting it in a collection bag kept in each ward. Second, doctors’ lists were identified using the electronic staff directory on our hospital intranet and sent via internal mail. Involved clinical specialties included: Accident and Emergency, Anaesthesia and Intensive Care, Clinical Oncology, Medicine and Therapeutics, Obstetrics and Gynaecology, Orthopaedics, Paediatrics, and Surgery. These clinical specialties were chosen as their staff are directly in contact with patients on a daily basis. Simple consecutive randomisation was carried out in distributing the questionnaires. For nurses, each ward was supplied equal numbers of both sets of vignettes and likewise for doctors in each specialty.
Statistical Analyses
Questions were devised to ascertain 4 main aspects, including social exposure, work exposure, negative experiences with psychiatric patients, and history of mental illness in their family and friends. The internal consistencies of the questions were calculated. The Cronbach’s alpha for questions gauging social exposure, work exposure, and negative experiences were 0.76, 0.42, and 0.61 respectively. Ordinal regression was carried out to examine factors affecting response to the 19 statements in the third part of the questionnaire. Social exposure, work exposure, negative experiences, years of working experience, sex, occupation, history of mental illness in the family and / or friends, case (i.e. vignette depicting a psychiatric patient) and control (i.e. vignette being a diabetes mellitus patient) being co-variants or factors in the regression. The Statistical Package for the Social Sciences (SPSS) Windows version 10.0 was used to analyse the data.
Results
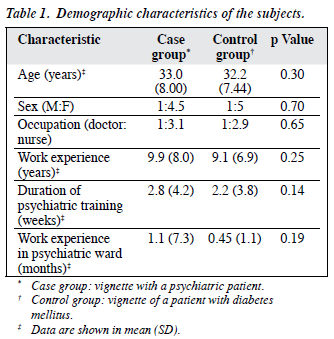
One thousand two hundred questionnaires were distributed, with equal numbers receiving the vignettes about the psychiatric patient (case group) and patient with diabetes (control group). A total of 190 (31.7%) subjects in the case group and 243 (40.5%) in the control group completed the questionnaire, yielding a total response rate of 36.1% (433/1200). The mean age of the respondents was 32 years; 74 (17.3%) were male, 354 (82.7%) were female, and 5 did not state their sex. In all, 107 (24.9%) were doctors, 322 (75.1%) were nurses, and 4 did not state their occupation. Their years of work experience ranged from 0.5 to 36 (mean, 9.5) years. Whereas 248 of the respondents had received no prior psychiatric training being 2.5 weeks. There were no statistically significant differences in demographic characteristics between the case and control groups (Table 1).
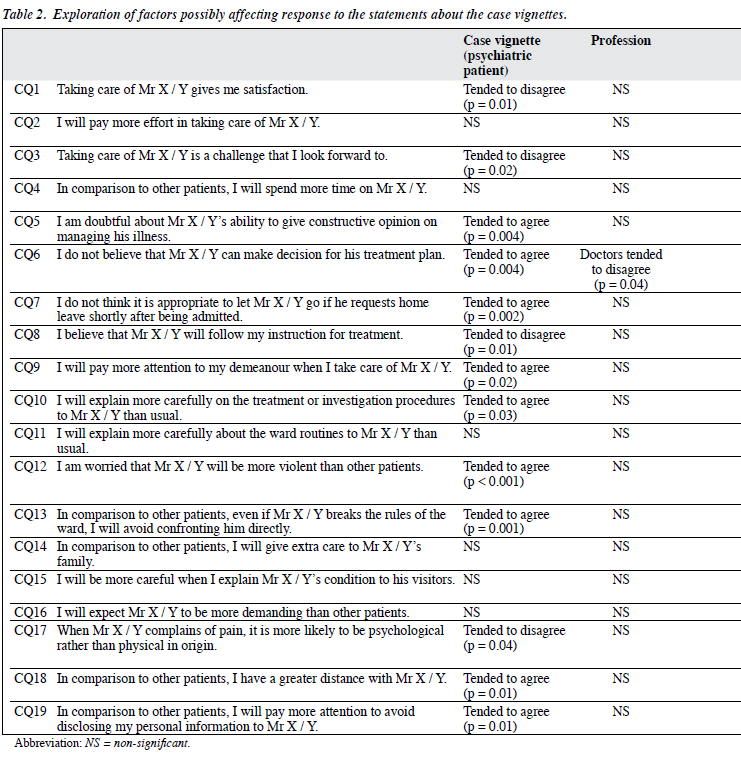
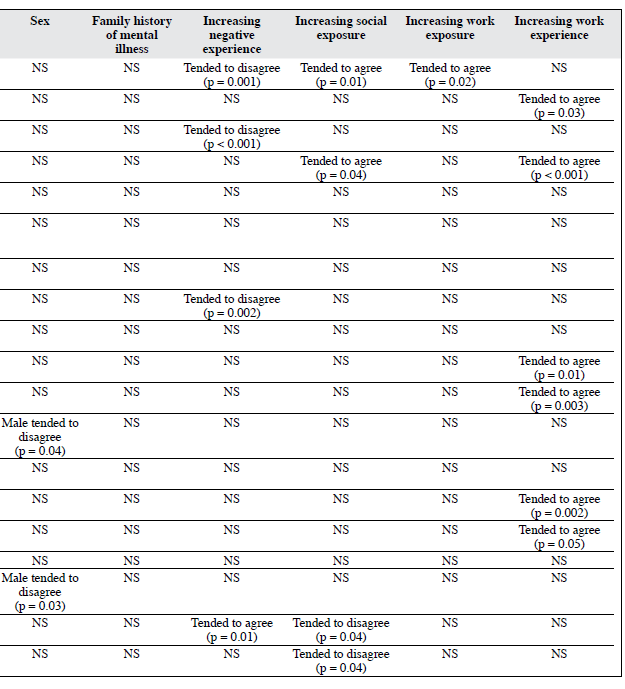
Factors affecting attitudes towards care of the subject in the case vignette are summarised in Table 2. According to the regression analysis, the diagnosis influenced opinions of the subjects towards the negative side. Healthcare workers were less likely to view the task of managing psychiatric patients as satisfying (CQ1) [p = 0.01] or challenging in a positive way (CQ3) (p = 0.02). Staff members with previous negative experiences with psychiatric patients were even less likely to do so (p < 0.001). Psychiatric patients were assumed to lack the capacity to give consent and make decisions regarding treatment options. The subjects contended that psychiatric patients lacked the ability to give constructive opinions about their treatment options (CQ5) [p = 0.004], make decisions about their treatment plans (CQ6) [p = 0.004], felt it was more inappropriate to concede to home leave requests after admission (CQ7) [p = 0.002], and considered that they were not able to follow treatment instructions (CQ8) [p = 0.01]. They also believed that psychiatric patients would be more violent than others (CQ12) [p < 0.001] and thus they tended to adopt a self- protective way of handling them and avoid unnecessary conflicts (CQ13) [p = 0.001].
An open-ended question was asked to explore each subject’s views about psychiatric patients. The most common responses in descending order of frequency were: “unstable”, “emotional”, “dull”, “difficult to understand”, and “pitiful”.
Discussion
This was the first local study to explore the attitudes of healthcare professionals towards psychiatric patients in a general hospital. To reduce observer and social desirability biases, we adopted an anonymous survey technique with case vignettes. The study was conducted in 1 general hospital in the territory only, and therefore the results should be interpreted with caution.
The usual assumption that healthcare professionals would have a more liberal and educated understanding about the relationship between mental illness and violence was not evident from this study. In the West, it is reported that 86% of stories in the newspapers dealing with mental illness focus on violence.32 Positive stories depicting recovery from the most serious mental illnesses were lacking. Social and work exposure, or negative experiences with psychiatric patients had no effect in terms of altering perceptions of psychiatric patients. As our subjects had fairly little contact with psychiatric patients, the chance of having an enriching experience was limited. Comparison of responses to those obtained from staff working in psychiatric units might yield a different picture.
When the psychiatric patient complained of pain, our subjects tended to think it had a physical rather than psychological origin, which was unexpected as the usual assumption would be that most physical complaints of psy- chiatric patients are psychological. There could be several reasons for this. First, diabetes mellitus is itself a chronic and disabling medical condition. The illness behaviours of patients with chronic medical illnesses (including diabetes mellitus, renal diseases, etc.) may be perceived by healthcare professionals as being demanding and manipulative, thus ascribing a lot of their somatic complaints as psychological in nature. Second, social desirability bias may operate, with subjects tending to give a ‘politically correct’ answer. Third, having depicted a psychotic patient with chronic symptoms in the case vignette, the subjects commonly described the patient as “crazy” but “honest”. Medical students and doctors in a university teaching hospital in London declared difficulty in communicating with psychiatric patients.33 This view was echoed in our study: psychiatric patients were described as “difficult to communicate with”. Although some mental disorders do impair the ability to communicate, most sufferers from mental disorders retain the capacity and desire to communicate.
Previous studies of stigma against psychiatric patients using subjects from the community as well as medical / dental students revealed that increasing personal contact with such patients increased the positive attitudes towards them.30,31 Our results echoed these findings, in that social exposure to psychiatric patients increased positive attitudes towards them. However, such personal contacts could also be a double-edged sword; positive experience may decrease negative attitudes and negative experience increase negative connotations. Arkar and Eker34 found that personal contact with persons having mental illness or having a mentally ill member in the family did not affect attitudes. Another study showed that the attitudes towards mental illness became less positive with increasing personal contact.20 Distinction between the qualities of the past experience was therefore important in formulating the attitudes.35 We found that an increase in negative experiences with psychiatric patients led to increased negative attitudes.
Previous research on strategies that could be used to diminish public stigma towards psychiatric patients identified 3 effective approaches, namely protest, education, and contact.36 Participation in education programmes also lead to a more positive attitude towards psychiatric patients.37,38 However, other studies had revealed contradictory views. A medical understanding of mental illness may lead to a paradoxical increase in social distance.17 We could not clarify this issue in our study, because of the extremely limited formal psychiatric training and experience that our subjects had received. Ideally, a study using a sample with more formal psychiatric training and experience might better address this issue.
We also noted that as the years of work experience increased, there was a more positive attitude towards patients in general, regardless of the nature of the case vignette. In our study, history of mental illness in families and friends did not have a statistically significant association with the opinions observed. The effect of this factor might have already been reflected in the degree of social exposure, instead of showing up in a “yes” or “no” response to the questions ascertaining these issues.
An alternative approach to understanding the attitudes of healthcare professionals towards psychiatric patients in a general hospital would have been through conducting focus groups. Our study might have been improved by holding focus group discussions to ascertain the validity of the questionnaire, before the survey was actually conducted. As in other surveys, non-respondents might form a very distinct group holding different opinions. In our case, the non- respondents may have held more negative attitudes towards psychiatric patients. Possible ways to further increase the response rate, such as distributing the questionnaire more than once or providing incentives could have be considered. The study was carried out in 1 regional hospital in Hong Kong, so extrapolating its findings to other general hospitals may not be appropriate. Other general hospitals could be recruited to conduct a larger-scale study to improve its validity.
Stigma towards psychiatric patients existed within the healthcare professionals in the general hospital we studied. The issue should be acknowledged and more clinical research is needed in this area to obtain an in-depth understanding of the phenomenon.
Acknowledgements
We would like to thank all those healthcare professionals who participated in this study.
References
- Corrigan PW. The impact of stigma on severe mental illness. Cogn Behav Pract 1998;5:201-22.
- Lawrie SM. Stigmatisation of psychiatric disorder. Psychiatr Bull Coll Psychiatr 1999;23:129-31.
- Manning C, White PD. Attitudes of employers to the mentally ill. Psychiatr Bull Coll Psychiatr 1995;19:541-3.
- Wahl OF. Mental health consumers’ experience of stigma. Schizophr Bull 1999;25:467-78.
- Druss BG, Rosenheck RA. Use of medical services by veterans with mental disorders. Psychosomatics 1997;38:451-8.
- Lawrie SM, Martin K, McNeill G, Drife J, Chrystie P, Reid A, et al. General practitioners’ attitudes to psychiatric and medical illness. Psychol Med 1998;28:1463-7.
- Dembling BP, Chen DT, Vachon L. Life expectancy and causes of death in a population treated for serious mental illness. Psychiatr Serv 1999;50:1036-42.
- Druss BG, Bradford DW, Rosenheck RA, Radford MJ, Krumholz HM. Mental disorders and use of cardiovascular procedures after myocardial infarction. JAMA 2000;283:506-11.
- Phipps L. Psychiatric evaluation and outcomes in candidates for heart transplantation. Clin Invest Med 1997;20:388-95.
- Corrigan PW, Matthews AK. Stigma and disclosure: implications for coming out of the closet. J Ment Health 2003;12:235-48.
- 1 Link BG, Yang LH, Phelan JC, Collins PY. Measuring mental illness stigma. Schizophr Bull 2004;30:511-41.
- Park RE. The concept of social distance. Journal of Applied Sociology 1924;8:339-44.
- Osgood CE, Suci GJ, Tannenbaum PH. The measurement of meaning. Urbana, IL: University of Illinois Press; 1957.
- Cohen J, Struening EL. Opinions about mental illness in the personnel of two large mental hospitals. J Abnorm Soc Psychol 1962;64:349-60.
- Taylor SM, Dear MJ. Scaling community attitudes toward the mentally ill. Schizophr Bull 1981;7:225-40.
- Angermeyer MC, Matschinger H. The effect of personal experience with mental illness on the attitude towards individuals suffering from mental disorders. Soc Psychiatry Psychiatr Epidemiol 1996;31:321-6.
- Lauber C, Nordt C, Falcato L, Rossler W. Factors influencing social distance toward people with mental illness. Community Ment Health J 2004;40:265-74.
- Stuart H, Arboleda-Florez J. Community attitudes toward people with schizophrenia. Can J Psychiatry 2001;46:245-52.
- Crisp AH, Gelder MG, Rix S, Meltzer HI, Rowlands OJ. Stigmatisation of people with mental illnesses. Br J Psychiatry 2000;177:4-7.
- Gathered A, Reid JJ. Public attitudes and mental health education: Northampton Mental Health Project 1963. Northampton: Northampton County Council; 1967.
- Angermeyer MC, Matschinger H. Social distance towards the mentally ill: results of representative surveys in the Federal Republic of Germany. Psychol Med 1997;27:131-41.
- Chou KL, Mak KY, Chung PK, Ho K. Attitudes towards mental patients in Hong Kong. Int J Soc Psychiatry 1996;42:213-9.
- Chou KL, Mak KY. Attitudes to mental patients among Hong Kong Chinese: a trend study over two years. Int J Soc Psychiatry 1998;44:215-24.
- Walt AP, Gillis LS. Factors that influence nurses’ attitudes toward psychiatric patients. J Clin Psychol 1979;35:410-4.
- Bailey SR. An exploration of critical care nurses’ and doctors’ attitudes towards psychiatric patients. Aust J Adv Nurs 1998;15:8-14.
- Jorm AF, Korten AE, Jacomb PA, Christensen H, Henderson S. Attitudes towards people with a mental disorder: a survey of the Australian public and health professionals. Aust N Z J Psychiatry 1999;33:77-83.
- Sevigny R, Yang W, Zhang P, Marleau JD, Yang Z, Su L, et al. Attitudes toward the mentally ill in a sample of professionals working in a psychiatric hospital in Beijing (China). Int J Soc Psychiatry 1999;45:41-55.
- Mukherjee R, Fialho A, Wijetunge A, Checinski K, Surgenor T. The stigmatisation of psychiatric illness: The attitudes of medical students and doctors in a London teaching hospital. Psychiatric Bull R Coll Psychiatr 2002;26:178-81.
- Liggins J, Hatcher S. Stigma toward the mentally ill in the general hospital: a qualitative study. Gen Hosp Psychiatry 2005;27:359-64.
- Chung KF, Chen EY, Liu CS. University students’ attitudes towards mental patients and psychiatric treatment. Int J Soc Psychiatry 2001;47:63-72.
- Lee S, Lee MT, Chiu MY, Kleinman A. Experience of social stigma by people with schizophrenia in Hong Kong. Br J Psychiatry 2005;186:153-7.
- Wahl OF, Wood A, Richards R. Newspaper coverage of mental illness: Is it changing? Psychiatric Rehabilitation Skills 2002;6:9-31.
- Mukherjee R, Fialho A, Wijetunge A, Checinski K, Surgenor T. The stigmatisation of psychiatric illness: the attitudes of medical students and doctors in a London teaching hospital. Psychiatr Bull R Coll Psychiatr 2002;26:178-81.
- Arkar H, Eker D. Influence of having a hospitalized mentally ill member in the family on attitudes toward mental patients in Turkey. Soc Psychiatry Psychiatr Epidemiol 1992;27:151-5.
- Desforges DM, Lord CG, Ramsey SL, Mason JA, Van Leeuwen MD, West SC, et al. Effects of structured cooperative contact on changing negative attitudes toward stigmatized social groups. J Pers Soc Psychol 1991;60:531-44.
- Corrigan PW, Penn DL. Lessons from social psychology on discrediting psychiatric stigma. Am Psychol 1999;54:765-76.
- Corrigan PW, River LP, Lundin RK, Penn DL, Uphoff-Wasowski K, Campion J, et al. Three strategies for changing attributions about severe mental illness. Schizophr Bull 2001;27:187-95.
- Holmes EP, Corrigan PW, Williams P, Canar J, Kubiak MA. Changing attitudes about schizophrenia. Schizophr Bull 1999;25:447-56.