Hong Kong J Psychiatry 2006;16:7-13
ORIGINAL ARTICLE
DM Tse, KK Wu, MH Suen, FY Ko, GL Yung
Dr Doris M Tse, FRCP, FHKAM (Medicine), Department of Medicine and Geriatrics, Caritas Medical Centre, Hong Kong, China.
Dr Kitty K Wu, PhD, M Soc Sc (Clinical Psychology), Department of Clinical Psychology, Caritas Medical Centre, Hong Kong, China.
Ms Margaret H Suen, MHA, BSW, Department of Medical Social Work, Caritas Medical Centre, Hong Kong, China.
Ms Fanny Y Ko, CPHQ, M Sc (Health & Hospital Management), Continuous Quality Improvement Team, Caritas Medical Centre, Hong Kong, China.
Ms Grace L Yung, RN, Department of Medicine and Geriatrics, Caritas Medical Centre, Hong Kong, China.
Address for correspondence: Dr Doris Man-Wah Tse, Department of Medicine and Geriatrics, Caritas Medical Centre, 111 Wing Hong Street, Shamshuipo, Kowloon, Hong Kong, China.
Tel: (852) 3408 7454; Fax: (852) 2148 4399;
E-mail: mwtse@ha.org.hk
Submitted: 11 May 2006; Accepted: 12 June 2006
Abstract
Objective: To study the perception of doctors and nurses on the care and bereavement support for relatives of critically ill and dying patients in an acute medical care setting.
Participants and Methods: A self-administered questionnaire survey was completed by 169 nurses and 20 doctors at the Department of Medicine and Geriatrics, Caritas Medical Centre, Hong Kong.
Results: When handling the reactions of bereaved relatives, the reported confidence of respon- dents did not agree with their ability to take the initiative. Nurses who perceived themselves as having no confidence would proceed to manage relatives' emotions. Familiarity with the proce- dures related to the death of a patient was not associated with staff initiative. Non-acceptance by relatives of a patient's death and strong emotions were reported to be most difficult factors to manage. The needs of the staff were identified for improvement of care.
Conclusion: When encountering the death of a patient, one-third of staff would not be confident and one-third would not take the initiative when managing relatives' emotions. Enhancement of knowledge and skills for doctors and nurses for providing support for bereaved relatives in an acute medical setting is indicated.
Key words: Death, Grief, Referral and consultation, Staff development
Introduction
In many developed countries, including Hong Kong, death is highly institutionalised. Health care workers have frequent exposure to death and dying, while family members of the deceased initially have to grieve in the unfamiliar environ- ment of the hospital. Family members have reported that emotional support both before and after a patient's death is an important determining factor in defining quality end-of- life care.1 Evidence shows that intervention for bereaved relatives results in a positive outcome for their psychologic- al well-being.2 Despite the importance of this issue and the potential benefits of managing death, health care workers are often not equipped to intervene with families facing the death of a relative.3
Bereavement care services are part of health care provi- sion in certain settings, but are highly variable in structure and content. For example, bereavement care is regarded as a component of a comprehensive palliative care service, and is well received by patients' relatives.4,5 The needs of relatives facing sudden or catastrophic death has also drawn the attention of health care workers in settings such as the Accident and Emergency Department, Intensive Care Unit, and Neonatal Unit.6-8 However, most hospital deaths occur in other settings. For example, in a typical acute general hospital in Hong Kong (Caritas Medical Centre), 75% of hospital mortality occurs in the acute general wards of the Department of Medicine and Geriatrics (DMG).
The needs of families whose relative has died in an acute care setting should not be ignored. In one study, bereaved families reported that doctors and other health professionals could have done something more to help them prepare for the death of a relative.3 There are reports addressing the importance of this issue, and practical guidelines for professionals have been suggested.9-12 Nonetheless, there are few studies on bereavement in acute care settings.1 This ques- tionnaire survey was conducted to explore the perception of doctors and nurses on the death of a patient and the level of support for bereaved relatives. The survey was part of a local programme initiated to enhance the awareness of the needs of bereaved people among doctors and nurses, and was approved by the Hospital Management Committee.
Participants and Methods
Participants
A self-administered questionnaire was sent out to 210 nurses and 30 doctors working in the DMG in August 2002. All questionnaires remained anonymous.
Questionnaire Development
The questionnaire was designed by an expert focus group comprised of a palliative care specialist, clinical psych- ologist, medical social worker, senior nursing officer in an acute ward, and an officer in quality improvement. The items generated were consolidated and the questionnaire was administered to 3 nurses to test for feasibility. The final questionnaire was completed after minor alterations to the phrasing. The questionnaire referred to the situation of a dying patient, and consisted of structured and open-ended questions in the following areas: common questions and concerns raised by relatives; difficult questions or situations encountered by staff; staff familiarity with procedures rela- ting to the death of a patient; staff attitudes towards dealing with grief; and areas for improvement and training needs.
Data Analysis
Responses to the open-ended questions were summarised into categories based on rational interpretation by a medical doctor and a social worker, both of whom had experience in caring for critically ill or dying patients. The number of participants responding to each category was counted. Descriptive analysis was used. Kappa statistics were used for detecting statistical significance when appropriate. A k value of > 0.4 was regarded as significant. Pearson chi-squared test was used to test for association. To reduce inflated type I error due to repeated testing of association, the level of significance (0.05) was adjusted by the Bonferroni method,13 and divided by 16, the number of Pearson chi-squared tests conducted to examine the associ- ation between familiarity with the procedures and whether a respondent had the confidence and initiation to deal with bereaved people. To be considered significant, the p value had to be < 0.003 within any of the subtests conducted.
Results
240 questionnaires were sent out to 210 nurses and 30 doctors. There were 189 respondents; 169 nurses (response rate, 80.5%) and 20 doctors (response rate, 66.7%). Among the doctors, 20% were senior grade, and 10% of nurses were senior grade.
Relatives' Questions and Concerns
Relatives' questions and concerns when a patient was critically ill and dying was an open-ended question. Their concerns were categorised and are shown in Table 1. The relatives' concerns were generally medical in nature, and included the clinical condition of the patient, cause of deterioration, and expected survival. Nurses commonly reported that relatives enquired about the presence of doctors. Paradoxically, relatives also had frequent enquiries about chances of unrealistic outcomes such as recovery and discharge from hospital.
More than two-thirds of staff reported that relatives were concerned about staff efforts to 'save' the patient and the time of death. Approximately one-third of staff reported that relatives were concerned about the appearance of the dead body, the handling of the dead body, and the procedures related to the death certificate and the funeral. Fewer staff reported relatives' concern for the following items: symp- tom control, whether the dying patient was still connected to them through touch or words, and whether the patient died in peace.
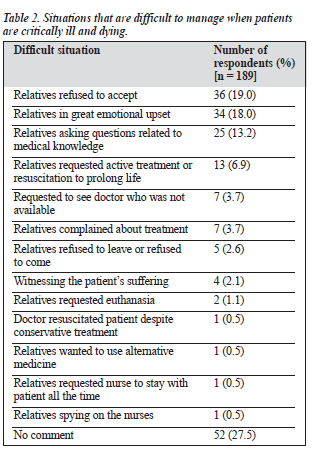
Difficult Situations for Staff
Situations that staff found difficult to deal with when patients were dying was an open-ended question. The situations reported were categorised and are summarised in Table 2. The difficulties faced by staff were related to the emotions of the relatives, most commonly their non- acceptance of the situation and the strong emotions ex- pressed such as crying loudly, shouting, or screaming, and displaced anger and aggression towards the staff. Nurses often felt helpless when relatives asked questions relating to the medical situation. It was also found to be difficult for staff when relatives requested futile life-sustaining treatment or cardiopulmonary resuscitation, either for prolonging life or while waiting for overseas family members to return. There was additional stress for nurses when doctors were not readily available. Some staff reported that witnessing the suffering of dying patients was the most difficult situation.
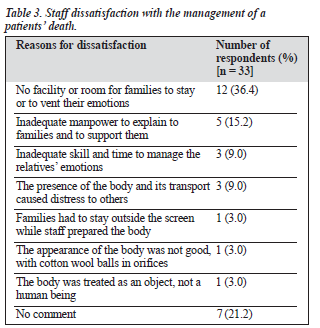
Staff Satisfaction with the Scene after a Death
Respondents were asked to report whether they were satis- fied with the management of the scene after the death of a patient. 183 staff responded, of whom 148 respondents (78.3%) were satisfied with the way they managed the scene and 33 respondents (17.5%) expressed dissatisfaction, for the reasons outlined in Table 3. Two doctors commented that this question was irrelevant, as they considered that their role was over after the death of a patient.
Attitude Towards Relatives' Grief
Respondents were asked to report whether they had con- fidence and initiative when dealing with the relatives' grief after a death. 170 patients responded (Table 4). There was no significant agreement between the confidence of the respondents and their initiative in dealing with grief (k = 0.26). Among the respondents who had no confidence in dealing with grief (n = 57), 23 (40.4%) would still initiate grief management; they were all nurses. None of the doc- tors who reported themselves as not being confident would initiate grief management.
Among the respondents who had confidence in grief management (n = 113), 34 (30.1%) would not take the initiative despite being confident. There was an open- ended question asking the participants for their reasons for taking or not taking the initiative in grief management; the answers are summarised in Table 5.
Respondents had to indicate whether they were familiar or unfamiliar with 8 standard procedures relating to the death of a patient (Table 6). All respondents answered this question. The procedure that most staff were familiar with was related to the practical procedures in the ward when a patient died (94.2%), while the least number of staff were familiar with the transport of the corpse to the funeral home (33.9%). For 4 of the 8 procedures, significant associations between familiarity and confidence were found. However, familiarity with procedures was not associated with initi- ation in grief management.
Areas for Improvement and Training Needs
Major areas for improvement included enhancing existing communication with relatives (47.6%), training in related areas (19%), improving the physical setting (14.8%), and providing counselling for dying patients and their families (10.6%).
Discussion
Death and dying is not an uncommon scene in a hospital, even when cure and recovery are the aim of treatment. How- ever, health care workers may not be well prepared to face death and to help dying patients and their families. Studies among nurses have shown that they often feel ill-equipped to provide support for relatives of patients who are dying.7,8 Likewise, physicians receive minimal training or guidance for the provision of bereavement support, despite the frequency with which physicians encounter bereaved families.9 In this survey, a satisfactory response rate was obtained from nurses and doctors. Strong emotions of the relatives and their non-acceptance of a patient dying were most commonly mentioned as difficult to manage and not all staff were prepared to handle relatives' emotions. In this survey, 113 of 170 staff (66.5%) were confident in manage- ment of grief and 102 of 170 staff (60%) would initiate grief management. However, staff confidence did not agree with their ability to initiate grief management; even staff with no confidence would proceed to initiate grief management, all of whom were nurses.
The reasons for taking the initiative in dealing with be- reaved relatives mostly stem from the nurses' conduct as caring and empathetic professionals. Two respondents ex- pressed the impact of their own personal experience of loss on their initiative to help bereaved relatives. Personal expe- rience of loss among professionals has been regarded as a potentially powerful way of bringing empathy to this issue.14 Reasons cited for not managing bereavement included lack of training, skill, experience, and time, and fear of making a mistake. Staff were frightened of the relatives' emotions and some admitted that they were afraid of facing their own emotions. Some respondents felt that grief should settle 'naturally'. Grief was felt to be a family affair, and a few doctors felt that their role ended when the patient died.
More than 90% of staff were familiar with the practical procedures in the ward as the patient died, while 75% of staff were familiar with the referral procedure for profes- sional support. While familiarity and knowledge of the prac- tical procedures may affect confidence, they had no signifi- cant relationship with initiative in managing grief. Profes- sional services can be utilised if staff identify bereaved people as being extremely distressed or demonstrating a ten- dency to self-harm. In one local study on the use of a liaison psychiatrist service in 1994, the findings suggested underuse of counselling services for bereaved people.15 Experience shows that referrals from acute wards for grief support are uncommon. The majority of bereaved families depend on the ward staff for grief management. Provision of structured training in grief management is needed for all acute care staff and may help to enhance their initiative by increasing their understanding of bereaved people.16 Enhancing aware- ness of the referral system for bereavement might improve the care of those relatives in need of help.
Although testing of the roles of doctors and nurses in grief management was not directly addressed in this study, findings of staff satisfaction with the management of the scene after a patient's death and confidence and initiation in managing relatives' grief suggest that doctors and nurses hold different assumptions of the role of offering bereave- ment support for relatives — nurses were more likely to assume an active and responsible role for managing grief than doctors. These findings would help to formulate a work- ing plan for improvement and to identify the training needs of staff for managing the death scene in a local setting.
This is the first local survey of critically ill dying patients. This survey had its limitations as respondents only in- cluded staff from the DMG. Although the study included responses from doctors, the number of doctors was too small for comparative analysis with the nurses. The results may be more representative for nurses than for doctors. There is a paucity of studies of the barriers to managing bereaved relatives in acute settings, although there are reports based on case studies and clinical experience of managing bereaved people,9 and on barriers to communication about end- of-life issues.17 The reliability and validity of categorising the response to open-ended questions was not formally established and verified. Results obtained from this study cannot be compared directly with other studies. However, the use of open-ended questions enabled respondents to freely express their views, which is essential for an ex- ploratory study.
Despite the limitations, the results of this survey have been helpful in highlighting the need for training for nurses and doctors, enhancement of the referral system for profes- sional support, advice on how to maintain the dignity of the deceased, and facilitating improvement in the mortuary setting. Heightened awareness of staff is needed to improve the death scene and managing the emotions of relatives in the acute care setting. Advocates for improvement in this area highlight the importance of the interdisciplinary team.2,18 It is recommended that a minimal level of care for bereaved relatives is desirable and justifiable.2
These results provide valuable information on how to improve the care of the relatives of dying patients in the acute care setting. More standardised and specific questions can be asked in future studies to examine the relationship between significant factors affecting the perception and behaviour of doctors and nurses in managing critically ill dying patients.
References
- Teno JM, Casey VA, Welch LC, Edgman-Levitan S. Patient-focused, family-centred end-of-life medical care: views of the guidelines and bereaved family members. J Pain Symptom Manage. 2001;22:738-51.
- Fauri DP, Ettner B, Kovacs PJ. Bereavement services in acute care settings. Death Stud. 2000;24:51-64.
- Barry LC, Prigerson HG. Perspectives on preparedness for a death among bereaved persons. Connecticut Med. 2002;66:691-96.
- Street AF, Love AW, Blackford J. Exploring bereavement care in inpa- tient settings. Contemp Nurse. 2004;17:240-50.
- Seamark DA, Williams S, Hall M, Lawrence CJ, Gilbert J. Dying from cancer in community hospitals or a hospice: closest lay carers' perceptions. Br J Gen Pract. 1998;48:1317-21.
- Ting SM, Li P, Lau FL, et al. Acute bereavement care in the emergency department: does professional-supported volunteers model work? Eur J Emerg Med. 1999;6:237-43.
- Granger CE, George C, Shelly MP. The management of bereavement on intensive care units. Intensive Care Med. 1995;21:429-36.
- Chan MH, Chan SH, Day MC. Nurses attitudes towards perinatal be- reavement support in Hong Kong: a pilot study. J Clin Nurs. 2003;12: 536-43.
- Prigerson HG, Jacobs SC. Care for bereaved patients: "All the doctors just suddenly go." J Am Med Assoc. 2001;286:1369-76.
- Casarett D, Kutner JS, Abrahm J; End-of-Life Care Consensus Panel. Life after death: a practical approach to grief and bereavement. Ann Intern Med. 2001;134:208-15.
- Kent H, McDowell J. Sudden bereavement in acute care settings. Nurs Stand. 2004;19:38-42.
- Main J. Management of relatives of patients who are dying. J Clin Nurs. 2002;11:794-801.
- Bland JM, Altman DG. Statistics notes: multiple significance tests: the Bonferroni method. Br Med J. 1995;310:170.
- Mazto ML, Sherman DW, Penn B, Ferrell BR. The End-of-Life Nurs- ing Education Consortium (ELNEC) experience. Nurse Educator. 2003; 28:266-70.
- Wong MT, Pan PC. Patterns of psychiatric referral and attendance at three different settings in Hong Kong. Int Psychogeriatr. 1994; 6:199-208.
- Zerbe KJ, Steinberg DL. Coming to terms with grief and loss. Can skills for dealing with bereavement be learned? Postgrad Med. 2000; 108:97-8.
- Anselm AH, Palda V, Guest C, et al. Barriers to communication re- garding end-of-life care: perspectives of care providers. J Crit Care. 2005;20:214-33.
- Rawlings D, Glynn T. The development of a palliative care-led memo-rial service in an acute hospital setting. Int J Palliat Nurs. 2002;8:40-7.