East Asian Arch Psychiatry 2006;16:27-33
ORIGINAL ARTICLE
BA Issa, O Baiyewu
Dr Baba Awoye Issa, FWACP, Department of Behavioural Sciences, College of Medicine, University of Ilorin, Nigeria.
Professor Olusegun Baiyewu, FWACP, FMCPsych, Department of Psychiatry, College of Medicine, University of Ibadan, Nigeria.
Address for correspondence: Dr Baba Awoye Issa, Department of Behavioural Sciences, College of Medicine, University of Ilorin, Nigeria.
Tel: (234 80) 5646 2071;
E-mail: issababa2002@yahoo.com
Submitted: 3 July 2006; Accepted: 6 September 2006
Abstract
Objective: To assess the quality of life of patients with diabetes mellitus and to determine the clinical and sociodemographic factors that affect the quality of life of these patients.
Patients and Methods: This was a cross-sectional study of 251 patients with diabetes mellitus attending the University of Ilorin Teaching Hospital, Nigeria. The World Health Organization quality of life instrument, short version and a sociodemographic questionnaire was adminis- tered to assess quality of life.
Results: Most of the respondents performed fairly well on the World Health Organization quality of life instrument, short version. Poor quality of life was associated with some of the physical compli- cations of diabetes mellitus, lower income, lower educational status, and type 2 diabetes mellitus. Conclusions: Lower income, lower education, low-rated employment, and physical complica- tions adversely affect the quality of life of patients with diabetes mellitus. Such factors need to be addressed by caregivers and physicians managing these patients.
Key words: Diabetes mellitus, Nigeria, Quality of life
Introduction
For most chronic illnesses, therapeutic success is traditionally measured by disease-free and overall survival, and control of major physical symptoms. While these factors play a primary role in such evaluations, efforts have been made to assess the extent to which chronic diseases and their treatments affect patients' functional capacity, psychological and social health, and overall sense of well-being or quality of life (QOL).1
The World Health Organization Quality of Life (WHOQOL) group defined QOL as an individual's perception of their position in life in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards, and concerns.2 This is a broad-ranging concept, affected in a complex way by a person's physical health, psychological state, level of independence, social relationships, and relationship to salient features of their environment.3
Diabetes mellitus is a typical chronic medical condition that places serious constraints on patients' activities. There is a need for extensive education and behaviour change to manage the condition. Lifestyle changes must incorporate careful dietary planning, eventual use of medication and, for all patients with type 1 diabetes and many with type 2 diabetes, the use of insulin and home blood glucose moni- toring techniques. Diabetes mellitus may lead to serious multisystem complications that often require additional in- trusive treatments. Diabetes mellitus is a useful model ill- ness for considering the effects of chronic disease on health- related quality of life (HRQOL).4
Studies have shown variability in the QOL effects of type 1 and 2 diabetes. For example, Gafvels found that patients with diabetes mellitus more frequently lived alone and re- mained childless, participated in fewer social activities, and indicated less personal satisfaction than control patients.5 Women appear to experience a greater impact of diabetes on their QOL and experience more worries about compli- cations and hypoglycaemia than men.6 Other studies have found that patients with diabetes mellitus have good QOL in comparison to those with some other chronic diseases and even to healthy populations.7 Mayou et al8 and Hanasted9 reported that the majority of patients with type 1 and type 2 diabetes mellitus experience a high degree of well-being, satisfaction, and enjoyment, although a minority noted that aspects of their lives were negatively affected by both forms of diabetes mellitus. It appears that type 1 diabetes mellitus has a greater negative impact on QOL than type 2 disease.10 These studies also indicated that the progression of diabetic complications is associated with a decrease in QOL.
The treatment of diabetes mellitus appears to have a complex effect on QOL. Jacobson et al found that patients with type 2 disease taking oral agents worried more about their condition than patients receiving insulin treatment or those treated by diet modification alone, suggesting the possibility that this transitional period was one in which the reality of having an illness was felt most intensely by patients.10 The same study also reported that insulin treat- ment of type 2 disease led to decreased satisfaction with HRQOL and greater impact of the illness. Mayou et al found little difference in the QOL between patients treated by diet, oral agents, or insulin therapy.8
Among patients with type I diabetes mellitus, HRQOL does not appear to be negatively influenced by the use of intensive treatment regimens. In the Diabetes Control and Complica- tions Trial, in which patients were randomly assigned to an intensive diabetic treatment regimen versus conventional treatment, QOL was not found to differ between the 2 groups during 6.5 years of follow-up.11 In addition, a recent study has demonstrated that early and aggressive intensive therapy leading to improved glycaemic control is likely to reduce the impact of diabetes mellitus on HRQOL by slowing the onset and progression of complications.12
QOL can be measured with generic or disease-specific instruments. The WHOQOL instrument, short version (WHOQOL-Bref) is a generic instrument with cross-cul- tural application and has been used as a measure of HRQOL for other chronic medical illnesses.2,13
There is a paucity of data on many aspects of diabetes care in the developing world and there are limited accounts of the relationship between diabetes mellitus and the prevailing social, economic, and cultural conditions and their impact on patients and patient care.14 This study attempts to improve on the data currently available from the developing world on QOL among patients with diabetes mellitus. The objective of this study was to assess the QOL of patients with diabetes mellitus and to determine the clinical and sociodemographic factors that affect their QOL.
Patients and Methods
The study was conducted at the endocrinology clinic of the University of Ilorin Teaching Hospital, Nigeria. The hospital is a tertiary centre that provides health services for Kwara State, one of the 36 States in Nigeria. The hospital also re- ceives referrals from towns and villages in the neighbouring states. The psychiatric unit of the hospital has 20 beds. Ad- equate liaison services exist between the various clinical departments of the hospital.
Patients
The patients were aged between 16 and 64 years. All pa- tients had diabetes mellitus and attended the endocrinology clinic of the hospital. Consecutive patients who met the inclu- sion and exclusion criteria were enrolled in the study.
Inclusion criteria were as follows:
- initially diagnosed with diabetes mellitus by the con- sultant endocrinologist and met the WHO criteria for diagnosis
- stable disease without need for hospital admission for 3 months prior to assessment
- established disease for at least 1 year.
Exclusion criteria included obvious damage to the brain or nervous system or any other concomitant disease that could affect the functions of the nervous system and inde- pendently affect reported or measured QOL. These criteria were used to ensure that the patients were already familiar with the dynamic of diabetes and to exclude other illnesses that would lead to poor QOL.
Measures
The instruments consisted of a questionnaire on socio- demographic and clinical history, and the WHOQOL-Bref.15 The WHOQOL-Bref is a 26-item self-administered generic questionnaire, being a short version of the WHOQOL-100 scale. This instrument emphasises the subjective response of patients rather than objective conditions. It was devel- oped in a wide range of languages for use in different cul- tural settings (including sub-Saharan Africa), and yields comparable scores across cultures. The WHOQOL is made up of domains (or dimensions) and facets (or subdomains). Domains are broad groupings (e.g., physical/psychological/social) of related facets. A facet is a specific aspect of life for which a coherent definition could be articulated. Of the 26 items of the WHOQOL-Bref, the items on 'overall rating of QOL' and subjective satisfaction with health are not included in the domains, but are used to form one facet on overall QOL and general health. In Nigeria, the WHOQOL-Bref has been used in previous studies of HRQOL.13,16-18 Each item of the WHOQOL-Bref has 5 options to which the patient is expected to respond on a 5-point Likert-type scale.
The WHOQOL-Bref produces a QOL profile with 4 do- main scores of physical health, psychological health, social relationships, and environment. There are 2 items that are examined separately: question 1 asks about an individual's overall perception of QOL; and question 2 asks about an individual's overall perception of their health. The 4 domain scores are scaled in a positive direction (higher scores de- note higher QOL). The scores of items within each domain are used to calculate domain scores. A score of mean ± 1 stan- dard deviation (SD) on each domain is graded 'fair', a score of < mean - 1 SD is 'poor', and a score of > mean + 1 SD is 'good'.13
Where more than 20% of data are missing from an assessment, the assessment was discarded and, where an item was missing, the mean of the other items in the do- main was substituted. Where more than 2 items were miss- ing from the domain, the domain score was not calculated (with the exemption of domain 3, where the domain should be calculated if £ 1 item is missing).2
All questionnaires were translated into Yoruba, the commonest language spoken in this area, and then back- translated to ensure equivalence and the Yoruba translation was administered to patients who did not speak English. The Yoruba translation has been validated and used in other studies and judged suitable and relevant for QOL studies in Nigeria.13
A pilot test of the instruments was performed among 10 patients to determine the acceptability, clarity, or ambiguity of the questionnaire items and identify logistical problems. The pilot study revealed that self-administration of the instruments might be inappropriate considering the varying levels of education of the patients. The instruments were therefore administered to the respondents by the author.
The permission of the hospital ethical committee was obtained and informed consent was obtained from all patients, following which the patients were administered the sociodemographic and WHOQOL-Bref questionnaires. Where applicable, references were made to the patients' case records and physical examinations of the attending physi- cians. The data were collected on clinic days during a 7-month period between December 2002 and July 2003.
Data Analysis
The Statistical Package for Social Sciences (SPSS) software (Version 11; SPSS, Chicago, IL, USA) was used for analysis. Summary scores were generated for the WHOQOL-Bref by organising the items into facets representing the domains covered by the questionnaire. Since the scores for each QOL domain were normally distributed, categorisation of levels of QOL for each domain was done using the mean value ± 1 SD. In computing these summary scores, patients with missing values were excluded from analysis for that particular domain. The categories of good, fair, and poor were cross- tabulated against patient variables such as age, sex, marital status, education, occupation, and clinical variables. Descrip- tive statistics were calculated for all variables. For continu- ous variables, these included mean ± SD. For categorical variables, descriptive statistics included the number and pro- portions in each category. Frequency distributions and cross tabulations were generated and chi-squared was used to compare proportions. Missing data were not considered in cross tabulations for the purpose of chi-squared calculation.
Results
267 consecutive attendees of the diabetes clinic met the in- clusion criteria during the course of the study. Of these, 251 patients (94%) consented to participate.
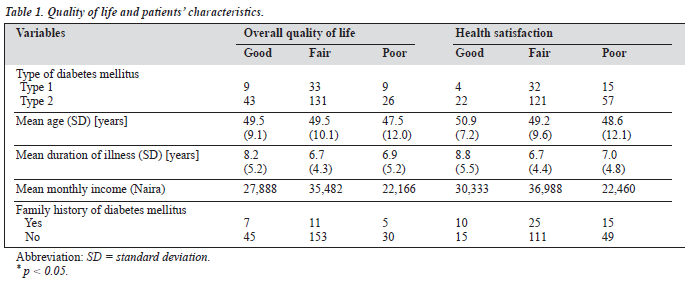
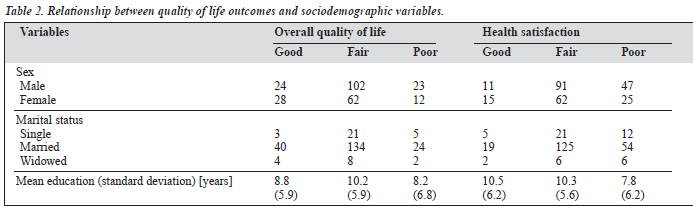
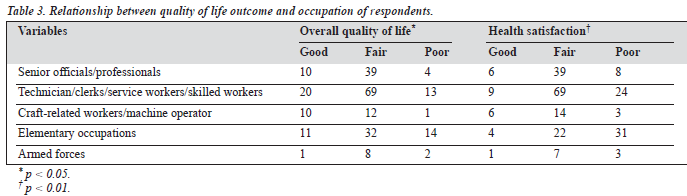
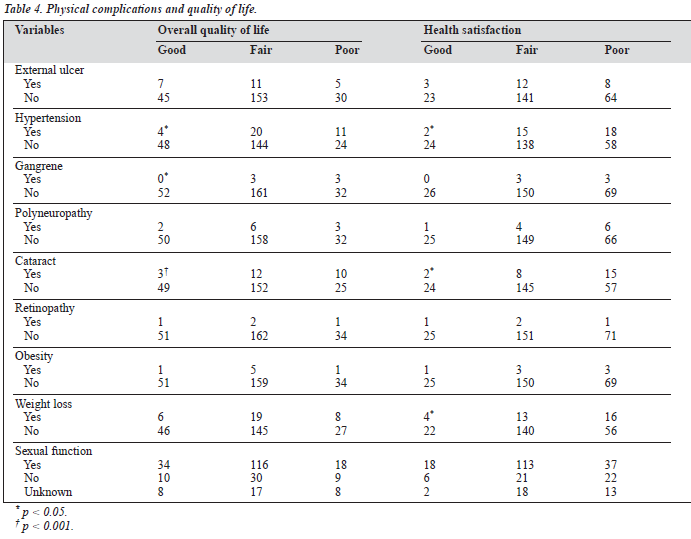
Fifty two patients (20.7%) had a good score, 164 (65.4%) had a fair score, and 35 (13.9%) had a poor score for overall QOL (Tables 1 and 2). Patients in the lower income bracket performed poorly on overall QOL. The occupation of re- spondents was statistically significantly related with this aspect of QOL. Respondents in elementary occupations (such as trading) were more likely to have a poor score for this domain (Table 3). The physical complications identi- fied as risk factors for a poor score were hypertension, gangrene, and cataract (Table 4).
Twenty six patients (10.4%) had good score, 153 (61.0%) had a fair score, and 72 (28.7%) had a poor score for health satisfaction. Occupation, particularly elementary occupation, cataract, hypertension, weight loss, sexual impairment, and lower income were related to a poor score.
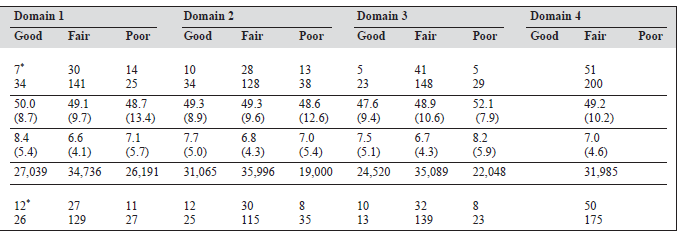
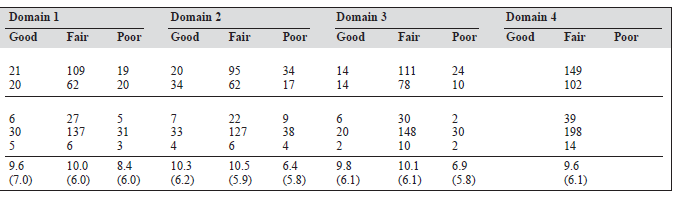
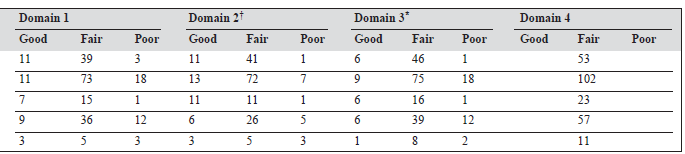
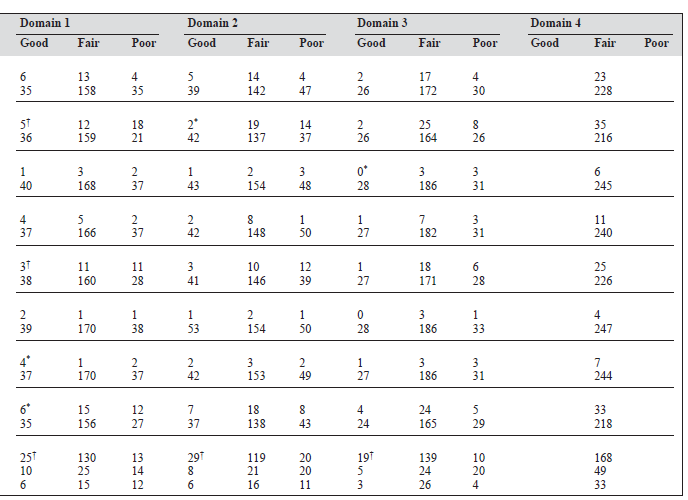
Forty one patients (16.3%) had a good score, 171 (68.1%) had a fair score, and 39 (15.5%) had a poor score for physi- cal health (domain 1). Occupation, hypertension, cataract, obesity, weight loss, impaired sexual function, and lower monthly income were significantly related with a poor out- come for the physical health domain.
Forty four patients (17.5%) had a good score, 156 (62.2%) had a fair score, and 51 (20.3%) had a poor score for the psychological domain (domain 2). Elementary occu- pation, hypertension, cataract, and lower monthly income were statistically related with a poor rating for this domain.
Twenty eight patients (11.2%) had a good score, 189 patients (75.3%) had a fair score, and 34 (13.5%) had a poor score for social relationships (domain 3). Impaired sexual function and lower monthly income were the factors associ- ated with poor outcome for this domain.
All 251 respondents had a fair score for the environment domain (domain 4).
Discussion
The QOL of patients with diabetes mellitus in this study was fairly good; approximately 1 of 7 patients rated poor for overall QOL while more than 6 of 10 and 1 of 5 rated fair and good, respectively. For health satisfaction, appro- ximately 3 of 10 patients rated poor, compared with 1 of 10 and 3 of 5 patients who rated good and fair, respectively. For the physical domain (domain 1), 3 of 20 patients rated poor. For the psychological domain (domain 2), 1 of 5 pa- tients rated poor. For social relationships (domain 3), only 1 of 15 patients rated poor, and all patients rated fair for environment (domain 4).
This study has shown that the QOL of patients with diabetes mellitus could be affected by the disease but supports the results of a previous study, which showed that patients with diabetes mellitus experienced a good QOL in comparison to other chronic disease groups and even to healthy populations.7 Hanasted reported that the majority of patients with type 1 and type 2 diabetes mellitus experience a high degree of well-being, satisfaction, and enjoyment, although a minority noted that aspects of their lives were negatively affected by both forms of diabetes.9
The mean educational level of patients who scored poor was generally lower than that for patients who scored good or fair. This is similar to the findings of Glasgow et al.19 This finding is important because education is an essential factor in understanding self care and management of diabetes, glycaemic control, and perception of self worth.
Overall QOL, health satisfaction, and the psychological and social domains are significantly correlated with occupation; patients who scored poor were more likely to have a low occupational status. Since lower occupation im- plies lower income, these patients need attention to break the cycle of low occupation status, low income, and poor QOL, which may be exacerbated among patients with chronic disease.
The finding in this study that patients with type 2 dis- ease are more likely to have a poor QOL contrasted with earlier findings that type 1 diabetes mellitus has a greater impact on QOL than type 2,4 although a previous study found little difference in the QOL of patients managed by diet, oral agents, or insulin therapy.8
Hypertension was statistically related to poor overall QOL, health satisfaction, physical health, and psychological domains. Gangrene also showed a significant relationship with overall QOL and social relationships. Cataract was re- lated to overall QOL and health satisfaction, while obesity was related only to the physical health domain. Weight loss was significantly associated with health satisfaction and the physical health domain. Patients with sexual function impairment had poor health satisfaction, physical health, psychological domain, and social relationships.
Poor QOL outcome was generally associated with lower monthly income. Association between physical complications and poor QOL has been noted by other researchers,20,21 and people with diabetes have a worse QOL than people with no chronic illness, but a better quality of life than people with other chronic diseases.22 Rubin and Peyrot also noted that the duration and type of diabetes are not consistently associated with QOL and that intensive treatment does not impair QOL.22 Complications of diabetes mellitus were re- ported to be the most important disease-specific determin- ant of QOL. Patients managed with insulin and those with microvascular complications were found to have a lower QOL than patients managed by diet and those without complications.23
The major limitations of this study are the cross- sectional design and its setting at a single centre, in that it may not be representative of patients with diabetes mellitus throughout Nigeria. As there are no previous studies on QOL of patients with diabetes mellitus using the WHOQOL-Bref in Nigeria, direct comparison with other studies is difficult. Life events and psychiatric disorders in the previous 2 weeks which could affect subjective QOL were not ruled out.
This study supports previous reports that QOL of patients with diabetes mellitus was fairly good. Poor QOL was associated with low occupational status and phy- sical complications, especially hypertension, gangrene, cataract, obesity, weight loss, and sexual function im- pairment. Other factors associated with poor QOL included non-insulin-dependent diabetes and low monthly income. Such factors therefore need to be addressed by health care workers and physicians managing patients with diabetes mellitus.
References
- Mirjam AG, Aaronson K. The role of health care providers and signifi- cant others in evaluating the quality of life of patients with chronic diseases: a review. J Clin Epidemiol. 1992;45:743-60.
- WHOQOL GROUP. The WHO quality of life assessment (WHOQOL): development and general psychometric properties. Soc Sci Med. 1998; 46:1569-83.
- Skevington SM, Lofty M, O'Connell KA. The World Health Organization's WHOQOL-BREF quality of life assessment: psycho- metric properties and results of the international field trial. Qual Life Res. 2004;13:299-310.
- Jacobson AM, DeGroot M, Samson JA. The effects of psychiatric dis- orders and symptoms on quality of life in patients with type I and type II diabetes mellitus. Qual Life Res. 1997;6:11-20.
- Gafvels C, Lithner F, Borjeson B. Living with diabetes: relationship to gender, duration and complications. A survey in northern Sweden. Diabet Med. 1993;10:768-73.
- Eiser C, Flynn M, Green E, et al. Quality of life in young adults with type I diabetes in relation to demographic and disease variables. Diabet Med. 1992;9:375-78.
- Stewart AL, Greenfield S, Hays RD. Functional status and well-being of patients with chronic conditions. JAMA. 1989;262:907-13.
- Mayou R, Bryant B, Turner R. Quality of life in non-insulin dependent diabetes and a comparison with insulin dependent diabetes. J Psychosom Res. 1990;34:1-11.
- Hanasted B. Self reported quality of life and the effect of different clini- cal and demographic characteristics in people with type I diabetes. Diabetes Res Clin. Pract. 1993;19:139-49.
- Jacobson AM, DeGroot M, Samson J. The evaluation of two measures of quality of life in patients with type I and type II diabetes. Diabetes Care. 1994;17:268-74.
- DCCT (Diabetes Control and Complications Trial) Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med. 1993;329:977-86.
- Jacobson AM. Impact of improved glycemic control on quality of life in patients with diabetes. Endocrin Pract. 2004;10:502-08.
- Olusina AK, Ohaeri JU. Subjective quality of life of recently discharged Nigerian psychiatric patients. Soc Psychiatry Psychiatr Epidemiol. 2003; 38:707-14.
- Kolawole BA, Abodunde O, Ikem RT, Fabiyi AK. A test of the reliabil- ity and validity of a diabetes specific quality of life scale in a Nigerian hospital. Qual Life Res. 2004;13:1287-95.
- World Health Organization. Program on mental health. WHOQOL- BREF: introduction, administration, scoring and generic version of the assessment. Geneva: World Health Organization; 1996.
- Fatoye FO, Komolafe MA, Adewuya AO, Fatoye GK. Emotional dis- tress and self-reported quality of life among primary care givers of stroke survivors in Nigeria. East Afr Med J. 2006;83:271-79.
- Makanjuola AB, Adeponle AB, Obembe AO. Quality of life in patients with schizophrenia in Nigeria. Nigerian Med Pract. 2005;48:36-42.
- Ohaeri JU, Olusina AK, Al-Abassi AM. Path analytical study of the short version of the WHO Quality of Life instrument. Psychopathology. 2006;39:243-47.
- Glasgow RE, Ruggiero L, Eakin EG. Quality of life and associated characteristics in a large national sample of adults with diabetes. Dia- betes Care. 1997;20:562-67.
- Shiu AT, Wong RY. Diabetes quality of life and associated characteris- tics of Hong Kong Chinese adults with diabetes. Proceedings of the 18th International Diabetes Federation Congress. August 24-29;2003. Paris, France.
- De Berardis G, Franciosi M, Belfiglio M, et al. Erectile dysfunction and quality of life in type 2 diabetic patients. Diabetes Care. 2002;25:284-91. 22.
- Rubin RR, Peyrot M. Quality of life and diabetes. Diabetes Metab ResRev. 1999;15:205-18.
- Bradley C, Todd C, Gorton T, Symonde E, Martin A, Plowright R. The development of an individualized questionnaire measure of perceived impact of diabetes on quality of life: the ADDQOL. Qual Life Res. 1999;8:79-91.