Hong Kong J Psychiatry 2008;18:55-61
Original Article
Depression among Secondary School Students: a Comparison between Urban and Rural Populations in a Malaysian Community
馬來西亞市區和農村地區中學生患抑鬱情況的比較
M Ramli, S Adlina, A Suthahar, AB Edariah, F Mohd Ariff, AHH Narimah, AS Nuraliza, I Fauzi, C Karuthan
Dr M Ramli, MMed (Psych), Faculty of Medicine, University of Technology MARA (UiTM), Shah Alam, Selangor, Malaysia.
Dr S Adlina, MPH, Faculty of Medicine, University of Technology MARA (UiTM), Shah Alam, Selangor, Malaysia.
Dr A Suthahar, MMed (Psych), Faculty of Medicine, University of Technology MARA (UiTM), Shah Alam, Selangor, Malaysia.
Dr AB Edariah, MPHTM, Faculty of Medicine, University of Technology MARA (UiTM), Shah Alam, Selangor, Malaysia.
Dr F Mohd Ariff, MPH, Faculty of Medicine, University of Technology MARA (UiTM), Shah Alam, Selangor, Malaysia.
Dr AHH Narimah, PhD, Faculty of Medicine, University of Technology MARA (UiTM), Shah Alam, Selangor, Malaysia.
Dr AS Nuraliza, PhD, Faculty of Medicine, University of Technology MARA (UiTM), Shah Alam, Selangor, Malaysia.
Dr I Fauzi, MMed (Psych), Department of Psychiatry, Selayang Hospital, Selayang, Selangor, Malaysia.
Dr C Karuthan, MSc (Applied Statistics), Faculty of Information Technology & Quantitative Sciences, University of Technology MARA (UiTM), Shah Alam, Selangor, Malaysia.
Tel: (603) 5544 3983 @ 6012 2484076; Fax: (603) 5544 2831; E-mail: ramlidr@yahoo.com
Submitted: 17 July 2007; Accepted: 23 August 2007
Abstract
Objective: To study the prevalence of depression among secondary schoolchildren in Selangor, and compare the same in urban and rural schools; also to identify factors associated with depression in secondary schoolchildren.
Participants and Methods: Two urban and 3 rural secondary schools were selected by 2-staged stratified random sampling, so as to represent the population of secondary schoolchildren in the state of Selangor, Malaysia. A total of 2,048 schoolchildren were enrolled and the level of depression was measured by a self-rated scale — the Children's Depression Inventory.
Results: The prevalence of possible depression in these students was 10.3%. There was no difference in the prevalence of significant depressive symptoms between rural and urban schoolchildren. Factors associated with depression were being female, Chinese, parents with low education level, stealing, and alcohol abuse (p < 0.001). Depression contributed significantly to suicidal tendencies (p < 0.001).
Conclusion: A sizable proportion of children in this secondary school population potentially suffered from depression. Psychological interventions are needed to ease this burden and ensure their well-being.
Key words: Adolescent; Depression; Prevalence; Students
摘要
目的:檢視在馬來西亞雪藺莪州學童患抑鬱的現患率, 把市區和農村學童作比較,且分析與中學學童患抑鬱的相關因素。
參與者與方法: 以兩個階段的分層隨機抽樣方法,於兩所市區和三所農村中學選出研究對象,代表雪蘭莪州的研究人口。合共2048名學童參與研究,並以自我評分的兒童抑鬱量表評估抑鬱程度。
結果:可能患抑鬱學生的現患率佔10. 3% 。農村和市區學童在明顯抑鬱症狀的現患率上並沒有分別。女性、華籍、父母有較低的教育水平、偷竊和翻酒( p < 0.001 )皆為患抑鬱的相關因素,也是導致有自殺傾向的明顯因素( p < 0 .001 ) 。
結論:是項研究中受抑鬱影響的兒童為數不少。減輕孩童病情和確保他們健康的心理治療是需要的。
關鍵詞:青少年、抑鬱、現患率、學生
Introduction
Childhood depression is a matter of major concern because of its prevalence, potential for recurrence, and impairment of functioning. Depressive episodes in childhood depression are recurrent and may lead to depression in adulthood, if the contributing factors remain unabated. Early depressive vulnerability is a predictive factor for depression in adulthood.1 Depressive disorders occur in approximately 2% of primary schoolchildren, and 4 to 8% of adolescents.2,3
About 45% of adolescents with major depression will relapse in young adulthood.4 Children and adolescents with depression are also at increased risk of suicide, substance use disorders, early pregnancy, poor academic performance, and impaired psychosocial functioning.5-7
Psychosocial problems associated with being depressed are relatively well known in adults. However, the extent to which these characteristics associate with depression in adolescents has received much less attention.8
Stressful life events, cognitive distortion, low self-esteem, increased self-consciousness, reduced social support, and impaired coping skills were among factors associated with depression.9,10 Although previous studies vary greatly in their methodology and focused on adults, sufficient convergence has emerged to implicate the following variables as potential risk factors for depression: previous history of depression; female gender; living in a dysfunctional family; low parental education; stressful life events and low social support; cigarette smoking; low self-esteem and body image; high self-consciousness; depression-related cognitions; school problems and reduced intellectual competence and coping skills; physical disability and poor physical health; excessive interpersonal dependence; problematic interpersonal behaviours; conflict with parents; and early death of a parent.11-14 Moreover, although many risk factors have been proposed and studied, relatively few have been examined systematically.
This study was undertaken because there is insufficient information pertaining to the mental health of Malaysian children. Not surprisingly, little has been mentioned regarding services to assist these children and their families, though they are invariably the main target of available social support systems. The main objective of this study was to determine the prevalence of clinically significant depressive symptoms among schoolchildren in Selangor and to compare urban and rural areas from this perspective. The study also aimed to determine factors associated with depression in these children.
Methods
Sampling Frame and Recruitment Centres
This was a cross-sectional pilot study to antedate a nationwide study across Malaysia. Selangor is one of the developed states in Malaysia, and was chosen for geographical and logistic reasons. According to the Department of Statistics of Malaysia, in 2000 about 30% of the 4.5 million Selangor inhabitants were adolescents. A 2-stage stratified random sampling was used to select the schools to represent Selangor schools, taking account of geographical factors relevant to urban and rural areas. The Ministry of Education gave full permission for the study to commence. Written consent was obtained from the parents and subjects after the procedures had been fully explained.
Subjects
In all, 2,048 students from 2 urban secondary schools (SMK Sri Permata and SMK Kelana Jaya, Petaling Jaya) and 3 rural secondary schools (SMK Sungai Pelek Sepang, Sekolah SMK Sri Tanjung Kuala Selangor, and SMK Sultan Abdul Aziz, Kuala Selangor) were selected to participate in the study. Inclusion criteria were ability to converse in English or Bahasa Malaysia, and provision of written consent to participate in this study.
Procedures
The Children’s Depression Inventory (CDI) is a self- administered questionnaire.15 The Bahasa Malaysia version of the CDI has been validated in Malaysia; it has a Cronbach’s alpha of 0.83, a sensitivity of 93%, and a specificity of 96% (personal communication, Rosliwati MY, 23 July 2007), indicating that it was a reliable and acceptable version. A cut-off point of 65 on T-score was used as recommended by CDI technical manual.15 Those who scored a T-score of 65 and above were considered possibly depressed. In the past, there were about 25 studies that used the CDI as a screening tool and it was widely demonstrated to be effective at differentiating between depressed and non-depressed children.15 Prior to the distribution of the questionnaire, the students were briefed and supervised by facilitators.
Statistical Analysis
Demographic data, severity of depressive symptoms, and factors associated with depression were analysed by Chi- square and general linear model procedures, using the Statistical Package for the Social Sciences (Windows version 11.0; SPSS Inc, Chicago [IL], US). The questionnaire also contained a few items measuring quality of relationships with parents, siblings, teachers, and schoolmates, and involvement in unwanted activities. These data were analysed by Chi-square tests.
Results
Socio-demographic Data
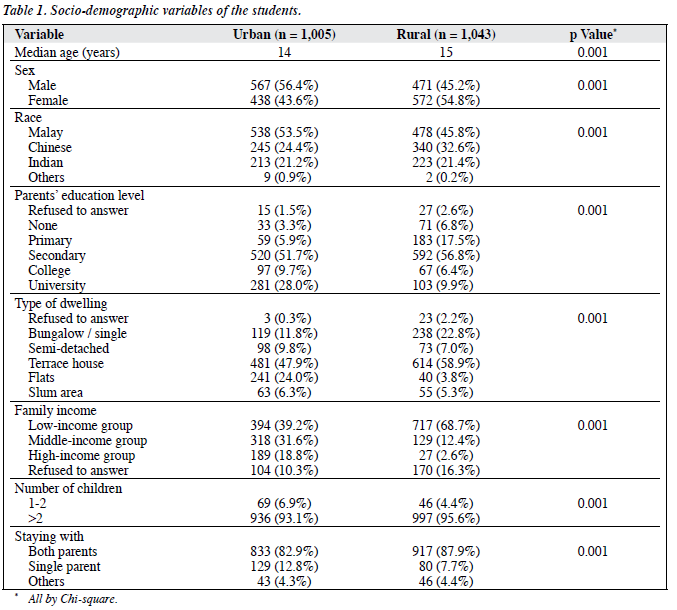
Table 1 shows the demographics in urban and rural students. All demographic variables revealed statistically significant differences (p < 0.05), especially with respect to socio- economic status (including family income levels and parental education), and consistent with expected differences.
Frequency of Possible Depression
Two hundred and eleven children (10.3%) scored a T-score of 65 and above on the CDI, and were considered screened- positive with respect to possible depression; 98 (9.8%) were urban students and 113 (10.8%) were rural students. However, further evaluation would be needed to confirm whether they fulfilled the criteria for major depressive disorder. The relative risks for urban and rural students being depressed were 0.90 (95% confidence interval [CI], 0.70-1.16) and 1.10 (95% CI, 0.88-1.25), respectively. There was no major difference in the prevalence of possible depressive cases in the urban and rural areas. According to CDI technical manual,15 the test has been used frequently as a screening tool for depression. Therefore we extrapolated that the prevalence of depression among the subjects was 10.3%. Further analysis of CDI subscales revealed that 9.2% of the subjects had negative mood, 5% had interpersonal problems, 8.3% had ineffectiveness, 4.6% had anhedonia, and 10.6% had negative self-esteem.
Factors Associated with Children’s Depression Inventory Scores
The general linear model univariate procedure was used to determine factors that were associated with depression among secondary schoolchildren. Based on Table 2, the mean CDI scores differ significantly between males and females, and with respect to races, parents’ education and income levels (p < 0.001), and the number of children in the family (p = 0.014). Further analysis showed that the mean depressive scores for females and Chinese as opposed to Malay and Indian students were significantly higher. There was no significant difference in scores between students of Malay, Indian, and other races. Those from lower socio-economic groups also had a higher mean score for depression. Students whose parents had no schooling or had primary schooling showed significantly higher mean scores compared to those whose parents had received secondary or tertiary education. Further analysis of the data showed that quality of relationships with parents, siblings, teachers, and schoolmates played a significant role in the pattern of CDI scores. The mean scores for depression were significantly higher in the group with poor relationships with parents, siblings, schoolmates, and teachers (p < 0.001).
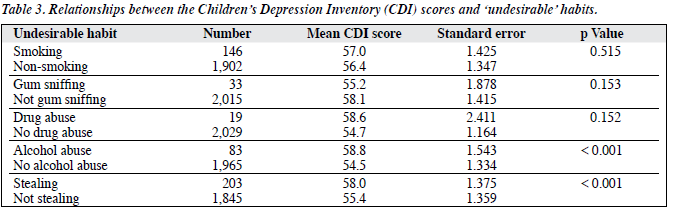
Five ‘undesirable’ habits were tested in this study (smoking, gum sniffing, drug abuse, alcohol abuse, and stealing). Of the 2,048 students, 7.1% were smokers, 1.6% were sniffing gum, 0.9% were involved in drug abuse, 4.1% took alcohol, and 9.9% were engaged in stealing. Table 3 shows the correlations between these habits and the level of depression; the mean CDI score for those imbibing alcohol was significantly higher than those who abstained. Similarly, those in the habit of stealing from others recorded significantly higher mean scores than those who did not. In conclusion, students who took alcohol and admitted stealing had significantly higher levels of depression than their peers. Although those who smoked and abused drugs had higher mean depression level scores, the differences were not statistically significant. Furthermore, the mean CDI scores increased with increasing level of suicidal tendency (p < 0.001).
Multivariate analyses of all confounders of depression revealed socio-economic variables such as parental income and level of education, number of siblings per family and type of dwelling, relationship with parent’s careers, and low self-esteem to be significant contributing factors for depression (Table 4).
Discussion
This study revealed that the prevalence of possible depression among the subjects was 10.3%, which is higher than the figure for all psychiatric morbidities obtained in Malaysian National Health and Morbidity Survey (8.7% for the state of Selangor).16 Another comparison by Kasmini et al17 in rural areas of Selangor (Jeram) revealed a rate of 15% as compared to 10.8% in this study (prevalence for the rural population in general). Thus, there appeared to be about a 4.2% fewer depressed subjects in rural Selangor after a 20-year interval. Several factors could explain this difference. First, the Reporting Questionnaire for Children was used in the two prior studies, while in the present study the CDI was used. The latter was cited in several studies in the past as a screening tool; substantially high scores indicate depression. Lowering the cut-off value reduces its sensitivity but increases specificity. In this study, a T- score of 65 or greater is used to identify possible depressive cases.15 Second, there was a considerable interval between this and the prior studies, which may explain the difference in prevalence for depression. Finally, the other 2 studies were conducted in the general population and looked at general psychiatric morbidities, whereas the present one focused only on secondary schoolchildren.
This finding was fairly similar to results from 2 other studies from Scandinavia and Italy18,19; in both studies, 10% of the children were depressed. In the United States, the prevalence of major depressive disorder was approximately 5 to 8% in adolescents.20 The prevalence of depression appeared to be increasing in successive generations of children, with onset at earlier ages.21
In this study, there was no major difference in the prevalence of possible depression between rural and urban students, though it was slightly higher in the former (10.8% vs 9.8%). Rutter et al,22 who undertook a vast population study comparing rural (Isle of Wight) and urban (Inner London) areas, found that the prevalence of depression in children was clearly higher in urban (13%) than rural areas (6-8%), possibly because the assessments were not conducted simultaneously in all schools. In particular, rural schools provided their data later, consistent with on-going events influencing the scoring of depression, especially major school examinations. Although there were no major examinations during the process of subject recruitment in our Selangor study, there were a few small tests for the rural students that might have influenced their mood.
In this study, girls were significantly more depressed than boys, which was consistent with other studies in the past. A study in Italy21 and another study by Chartier and Lassen 23 found that girls had significantly more depressive than boys. Another report from Brazil24 suggested significantly more females than males had scores above the cut-off point for depression (72.3% vs 27.7%), as did a study among Chinese secondary schoolchildren in Hong Kong (aged 13-17 years).25 Regardless of age, females are generally more susceptible to depression, due to patterns of help-seeking behaviours and multiple life events. Before the age of 13 years, the prevalence of childhood depression was equal between genders, but increased significantly in females after they reached the age of 14 years,26 although this was not a uniform finding. In studies by Finch et al27 and Huntley et al,28 boys were significantly more depressed than girls based on the CDI. Among the races, Chinese recorded a significantly higher mean T-score compared to other races (Malays, Indians, and others). In Malaysia, Chinese generally had higher socio-economic status as well as higher income level than others. The prevalence of depression should therefore have been lower. Our contrary findings might be due to Chinese individuals being more open about revealing their feelings than others.
In major epidemiological studies, prevalence of depression was found to be much higher among adolescents of low socio-economic status.3,14 The indicators of low socio-economic status were low levels of parental education, low parental income, and high economic burdens, such as high number of siblings per family. This study found that students with the above-mentioned factors were significantly more depressed. Depression among adolescents was also significantly associated with family dysfunction (single parents, divorced parents29) and poor social support.30
Prior studies concluded that between 25% and 32% of children who had lost one or both parents due to death, divorce, or separation were depressed.30,31 Our study also revealed that students who had poor relationships with their social network such as family, schoolmates, and teachers were more depressed. However, surprisingly the level of depression was not influenced by factors such as whether they stayed with one or both parents, though whether they were divorced was not specifically addressed. In Malaysia, it is quite common for fathers in rural areas to leave their families, to seek better-paid jobs in a big city or urban area, whilst still retaining emotional ties and supports for their families.
Students involved in drinking alcohol and stealing had significantly higher levels of depressive symptoms than those who were not, and those who smoked and took drugs also had higher mean scores for depression, but the latter differences were not statistically significant. In other studies, substance use has been recorded in approximately 25% of adolescents with depression.25,32 Depressed adolescents had a tendency to express their emotional incompetence by displaying externalising behaviours such as substance abuse.
Not surprisingly, those who were depressed were more prone to suicidal thoughts compared to those who were not. Suicide has become a growing public health concern, as successive generations have shown a parallel increase in suicide and depression in the paediatric age-group.10,21
Another study conducted on 79 male and 44 female inpatient children (aged 6-13 years) found that suicidal ideations were reported significantly more often among those with high depressive levels, high levels of hopelessness, and low self- esteem.33 Depression as measured by the CDI was the single best predictor of suicidal ideation and suicidal attempts.34
This study, which used a self-rated questionnaire only, did not entail second party verification of the depressive symptoms. In studies involving children, it is generally recommended to obtain second opinions, especially from parents or teachers. In acquiring information from children, they are bound to have recall bias, which includes misreporting or underreporting of symptoms. This issue should be highlighted and overcome in future larger studies so as to minimise recall bias. The validity of the Malay version is yet to be ascertained on a larger scale in the future. However our limited data show that its validity and reliability was good. There is also an issue regarding the validity of acquiring data about involvement in drugs via single party information (without further verification from parents). Other confounders such as recent adverse life events might hinder the results and was not looked into in this study. Recent life events such as parental loss and examinations influence children in particular, and could have a strong psychological impact. Researchers who are interested in this area should replicate this investigation, and include more questions on adverse life events.
The high frequency of possible depression in this population requires therapeutic and preventive interventions, and parents, teachers, and health care providers should heed the problem. Crucially, undiagnosed childhood depression may lead to various long-term, detrimental psychosocial consequences such as substance abuse, school dropout, suicide, and depression in adulthood. Childcare providers must be equipped with knowledge, attitudes, and skills to help these children cope with their emotions and stresses. In particular, ‘difficult children’ or those involved with disciplinary or conduct problems might be suffering from childhood depression.
Acknowledgements
We wish to extend our heartfelt gratitude to all students who participated in this study and to all their dedicated teachers for their cooperation.
References
- Petersen AC, Compas BE, Brooks-Gunn J, Stemmler M, Ey S, Grant KE. Depression in adolescence. Am Psychol 1993;48:155-68.
- Lewinsohn PM, Clarke GN, Seeley JR, Rohde P. Major depression in community adolescents: age at onset, episode duration, and time to recurrence. J Am Acad Child Adolesc Psychiatry 1994;33:809-18.
- Kessler RC, Walters EE. Epidemiology of DSM-III-R major depression and minor depression among adolescents and young adults in the National Comorbidity Survey. Depress Anxiety 1998;7:3-14.
- Lewinsohn PM, Rohde P, Klein DN, Seeley JR. Natural course of adolescent major depressive disorder: I. Continuity into young adulthood. J Am Acad Child Adolesc Psychiatry 1999;38:56-63.
- Brent DA, Baugher M, Bridge J, Chen T, Chiappetta L. Age- and sex- related risk factors for adolescent suicide. J Am Acad Child Adolesc Psychiatry 1999;38:1497-505.
- Rhode P, Lewinsohn PM, Seeley JR. Comorbidity of unipolar depression: II. Comorbidity with other mental disorders in adolescents and adults. J Abnorm Psychol 1991;100:214-22.
- Lewinsohn PM, Rohde P, Seeley JR, Klein DN, Gotlib IH. Natural course of adolescent major depressive disorder in a community sample: predictors of recurrence in young adults. Am J Psychiatry 2000;157:1584-91.
- Barnett PA, Gotlib IH. Psychosocial functioning and depression: distinguishing among antecedents, concomitants, and consequences. Psychol Bull 1988;104:97-126.
- Allgood-Merten B, Lewinsohn PM, Hops H. Sex differences and adolescent depression. J Abnorm Psychol 1990;99:55-63.
- Hops H, Lewinsohn PM, Andrews JA, Roberts RE. Psychosocial correlates of depressive symptomatology among high school students. J Clin Child Psychol 1990;19:211-20.
- Kandel DB, Davies M. Adult sequelae of adolescent depressive symptoms. Arch Gen Psychiatry 1986;43:255-62.
- Hammen C, Adrian C, Hiroto D. A longitudinal test of the attributional vulnerability model in children at risk for depression. Br J Clin Psychol 1988;27:37-46.
- Lewinsohn PM, Hoberman HM, Rosenbaum M. A prospective study of risk factors for unipolar depression. J Abnorm Psychol 1988;97:251- 64.
- Velez CN, Johnson J, Cohen P. A longitudinal analysis of selected risk factors for childhood psychopathology. J Am Acad Child Adolesc Psychiatry 1989;28:861-4.
- Maria K. Children’s Depression Inventory (CDI) technical manual. Main features of CDI. New York: Multi-Health Systems, Inc.; 2003:1- 7.
- National Health and Morbidity Survey in Malaysia. 1996. Institute of Public Health, Ministry of Health, Malaysia, 1997. In: Advocacy in action. The Globe Issue 1. Kuala Lumpur.
- Kasmini K, Ohn Kyaw, Hassan Almashoor S, Ramli H, Saroja K. Prevalence Study of Child Psychiatric Disorders in Malaysian Village. Jurnal Perubatan Universiti Kebangsaan Malaysia 1987;9:11-20.
- Arnarson EO, Smari J, Einarsdottic H, Jonasdottir E, The prevalence of depressive symptoms in preadolescent school children in Iceland. Scand J Behav Ther 1994;23:121-30.
- Poli P, Sbrana B, Marcheschi M, Masi G, Self-reported depressive symptoms in a school sample of Italian children and adolescents. Child Psychiatry Hum Dev 2003;33:209-26.
- Jellinek MS, Snyder JB, Depression and suicide in children and adolescents. Pediatr Rev 1998;19:255-64.
- Klerman GL, Lavori PW, Rice J, Reich T, Endicott J, Andreasen NC, et al. Birth-cohort trends in rates of major depressive disorder among relatives of patients with affective disorder. Arch Gen Psychiatry 1985;42:689-93.
- Rutter M, Yule B, Quinton D, Rowlands O, Yule W, Berger W. Attainment and adjustment in two geographical areas: III—Some factors accounting for area differences. Br J Psychiatry 1975;126:520- 33.
- Chartier GM, Lassen MK. Adolescent depression: children’s depression inventory norms, suicidal ideation, and (weak) gender effects. Adolescence 1994;29:859-64.
- Bahls S. Epidemiology of depressive symptoms in adolescents of a public school in Curitiba, Brazil. Rev Bras Psiquiatr 2002;24:63-7.
- Chan DW. Depressive symptoms and perceived competence among Chinese secondary school students in Hong Kong. J Youth Adolesc 1997;26:303-19.
- Costello EJ, Pine DS, Hammen C, March JS, Plotsky PM, Weissman MM, et al. Development and natural history of mood disorders. Biol Psychiatry 2002;52:529-42.
- Finch AJ Jr, Saylor CF, Edwards GL. Children’s depression inventory: sex and grade norms for normal children. J Consult Clin Psychol 1985;53:424-5.
- Huntley DK, Phelps RE, Rehm LP. Depression in children from single- parent families. J Divorce 1987;10:153-61.
- Fleming JE, Offord DR. Epidemiology of childhood depressive disorders: a critical review. J Am Acad Child Adolesc Psychiatry 1990;29:571-80.
- Monroe SM, Bromet EJ, Connell MM, Steiner SC. Social support, life events, and depressive symptoms: a 1-year prospective study. J Consult Clin Psychol 1986;54:424-31.
- Siegel K, Karus D, Raveis VH. Adjustment of children facing the death of a parent due to cancer. J Am Acad Child Adolesc Psychiatry 1996;35:442-50.
- Mattison RE, Handford HA, Kales HC, Goodman AL, Mc Laughlin RE. Four-year predictive value of the Children’s Depression Inventory. Psychol Assess 1990;2:169-74.
- Marciano PL, Kazdin AE. Self-esteem, depression, hopelessness and suicidal intent among psychiatrically disturbed inpatient children. J Clin Child Psychol 1994;23:151-60.
- Kazdin AE. French NH, Unis AS, Esveklt-Dawson K, Sherick RB. Hopelessness, depression, and suicidal intent among psychiatrically disturbed inpatient children. J Consult Clin Psychol 1983;51:504-10.