Hong Kong J Psychiatry 2000;10(3):27-36
ORIGINAL ARTICLE
RMK Ng & SP Leung
Abstract
There is limited data on the outcome of non-Western patients with chronic psychiatric illness discharged from psychiatric hospitals. Most outcome studies focus on psychiatric outcomes of relapse and mortality rates. In Hong Kong, there is no data on the long-term outcome of chronic patients discharged into the community.
The study investigated the multiple psychosocial aspects of chronic psychotic patients after 5 years of re-settlement in the community. A retrospective cross-sectional survey of a group of chronic psychotic patients discharged from a rehabilitation unit in a psychiatric hospital into the community used multiple scales to assess the physical, psychiatric and social well being of these patients.
Only two-thirds of patients remained in the community and 10% died due to medical problems. Patients frequently changed their place of residence. There was no incidence of major violence to the community. Only 30% remained in competitive employment. Most patients had multiple and severe social disabilities. In order to help patients fully re-integrate into the community, measures must be taken to alleviate the multiple social disabilities.
Key words: Chronic; Community; Outcome; Psychotic
Introduction
Quality of life research has become increasingly dominant in recent years because of the rising importance of consumerism.1
The concept of quality of life is understood by everyone and thus serves as a potential common language in the health care community.2 However, most quality of life measurements tend to emphasise subjective experience and neglect other potential confounders.3 Katschnig has demonstrated how a depressive state may distort the subjective reports of material and social living environments.3 Becker has argued that quality of life assessment should be carried out not only via the patient but also via professionals and key carers.4 He therefore devised the Wisconsin Quality of Life Index (W-QLI) with a professional and a carer version. Barry and Crosby have shown that hospitalised schizophrenic patients re-settled in the community showed little satisfaction despite objective improvement in living standard and leisure activities.5 Chronic schizophrenic patients also tend to overestimate their level of functioning and environmental assets, while depressive patients tend to underestimate both.6 A single composite scale of quality of life is simple to understand but the different areas of needs and deficits tend to be overlooked.
Against such a background, Katschnig argued that the concept of quality of life in psychiatry was only meaningful if the assessment was performed in a differentiated way which included interaction with the environment.3 He recommended the following guidelines:
- At least three assessments should be carried out, one by the patient, one by a professional and one by a family member or a friend.
- Three components should be distinguished
- subjective quality of life
- functioning in social roles
- external living conditions. - Different life domains should be assessed separately, since a person’s quality of life may be excellent in one and inferior in another. Intervention should aim at those areas of need.
- The inclusion of psychopathological symptoms should be made explicit.
- The assessment of quality of life needs to bear in mind the change in different components of well being, functional status, and environmental factors. There is also a possible downward drift of standards when comparing the actual situation and normal standards.
This study is an attempt to provide a close and comprehen- sive view of the quality of life of the study group in accordance with Katschnig’s model.
METHODS
This study attempted to look at the quality of life from the psychopathological dimensions, social role functioning, physical health, work status, income, objective and subjective environment, and social network, as well as the met and unmet needs in the community. This was a research project that combined the efforts of psychiatrists, nurses, and occupational therapists from the hospital pre-discharge unit at Castle Peak Hospital.
STUDY POPULATION
Castle Peak Hospital is the largest mental hospital in Hong Kong with 1741 beds, of which approximately 70% are for extended care patients.7 The hospital pre-discharge unit was set up in April 1993 as a hospital rehabilitation unit to facilitate chronic psychiatric patients for discharge back into the community. All these patients had been ill for a number of years and have no supportive relatives. Fifty one patients (40 males and 11 females) have successfully been discharged into halfway houses after a variable period of rehabilitation in the unit between April 1993 and March 1994, inclusive.
The sample had a mean age of 38.6 years (males, 38.2 years; females, 38.8 years). They were all chronic psychotic patients suffering from major psychosis for 12 years (mean, 11.8 years) and had been hospitalised in Castle Peak Hospital for approximately 5 years prior to discharge (mean, 5.3 years). They had an average of six episodes of admission to psychiatric facilities since the onset of illness, totalling a mean of 38.4 months in psychiatric facilities. They received rehabilitation in the hospital pre-discharge unit for a mean of 9.6 months before discharge. All had no supportive relatives who could provide home placement upon discharge. All were unemployed for at least 1 year prior to this episode of hospitalisation.
Letters explaining the purpose of the study were sent to individual non-governmental organisations. The halfway houses run by the different organisations were then contacted individually to trace the discharged patients. Verbal consent by the patients was initially obtained by telephone, with informed consent obtained during the first visit by the research staff. For patients who had been discharged home or re-housed compassionately after a stay in halfway houses, halfway house staff would first contact the individual patient to briefly explain the study. If the patient agreed, the research staff would contact the patient by telephone and arrange the first visit. For patients who refused to enter the study after the brief explanation by the halfway house staff, a letter was sent to the patients’ residence, explaining the aim of the study in detail and ensuring anonymity. For patients who lost contact with halfway houses, an effort was made to check the admission and in-patient records of all psychiatric units in Hong Kong.
A positive reinforcement of HK$150 was provided for each patient, who consented to participate in the study, in order to encourage them to complete all the schedules. This was necessary in view of the fact that it took a total of 6 hours for each patient to complete all the schedules. Furthermore, the study was usually performed outside working hours.
CLINICAL ASSESSMENT
A team of one psychiatrist, two registered psychiatric nurses and three occupational therapists visited each patient three times to administer each of the following schedules once. The study lasted for a period of 5 months from February 1998 to August 1998.
Demographic and work data
Information of the patients’ gender, ethnicity, and marital status, as well as their admission records were collected. These data were obtained from patients and confirmed by checking the old case notes. Details of contact with psychiatric and forensic services were also obtained. A work history and analysis for m was used by an occupational therapist to document a detailed work history.
Mental State Examination
Mental health contributes to the overall quality of life. It also serves to identify possible psychopathological fallacies that may affect the ratings in other life domains such as social network and unmet needs. All patients wer e administered the Structured Clinical Interview of DSM IV (SCID-IV).8 The rater (RN) was trained in SCID-IV via video training. The current severity of psychiatric symptoms were measured by 24-item Brief Psychiatric Rating Scale (BPRS)9 and by the Schedule for Assessment of Negative Symptoms (SANS).10 Both schedules were done by the psychiatrist (RN), who received video training in the use of the schedules. The inter-rater reliability with psychiatrists at Castle Peak Hospital was shown to be good, with a kappa coefficient for BPRS of 0.88 while that for SANS was 0.84 (p < 0.001).
Physical Health
Since poor health reduces quality of life, the physical health index (PHI) was used.11 This schedule was completed by the psychiatrist (RN).
Quality of the environment
The Environmental Index (EI) measures the degree of re- strictiveness of care setting.11 The Living Unit Environment Schedule measures the state of repair and attractiveness of the environment. The EI was administered to the sample by the three research occupational therapists. They achieved an inter-rater r eliability of kappa coefficient of 0.92 (p < 0.001).
Social Integration
The Social Network Schedule (SNS) was used in this study and was administered by three occupational therapists.12 Two research nurses administered the schedule to the study patients. The two nurses had an inter-rater reliability of kappa coefficient of 0.86 (p < 0.001)
Social Role Functioning
The Groningen Social Disabilities Schedule (GSDS) was used to measure the social disabilities in the sample group.13 The research psychiatrist attained an inter-rater reliability with a Chinese psychiatric colleague of kappa coefficient of 0.86 (p < 0.001).
Needs Assessment
The Camberwell Assessment of Needs (CAN; Research Version) was used.14 The two research nurses administered the CAN to all sample patients. The inter-rater reliability of kappa coefficient was 0.96 for staff rating and 0.97 for patient rating (p < 0.001)
RESULTS
PATIENTS’ CHARACTERISTICS
Of the 51 patients who were discharged during April 1993 to March 1994, 35 subjects were interviewed. Five male and two female subjects refused to be interviewed after a lengthy explanation by telephone and letters. Five patients could not be traced. Four subjects died due to medical illnesses but the exact medical cause was not known. There were no suicides, or violent or accidental deaths. Excluding the four patients who died, 75% of the original group were followed up.
All the patients who could not be traced were male. However, there were no statistical differences between the study group, those who refused to enter the study, and those who could not be traced in terms of age, diagnosis, and duration of hospitalisation prior to discharge from the hospital pre-discharge unit. However, patients who refused to enter the study or who could not be traced had all left the halfway house placement.
There was a predominance of male patients in this sample (74% male vs 26% female). They were mostly single or divorced (80%). They were all ethnic Chinese and 42% were born locally in Hong Kong. The mean age was 41.5 years for males and 41.8 years for females. The study group consisted of chronic psychiatric patients who had been ill for a number of years (mean duration of illness, 22.6 years for males and 24.8 years for females).
CURRENT COMMUNITY PLACEMENT
Five years after discharge from Castle Peak Hospital, 14 patients (40%) remained in halfway houses and 10 patients (28.6%) moved out to live on their own. During the study period, nine patients (26%) were re-hospitalised with a mean duration of stay in the psychiatric hospital of 51.4 weeks (SD 36.1 weeks). There was a trend towards significance (p < 0.1) in terms of the difference in the duration of mental illness and episodes of hospitalisation between in-patients and out-patients. There was no statistically significant difference in terms of number of jobs held previously or number of friends or confidants (p > 0.1).
MENTAL HEALTH
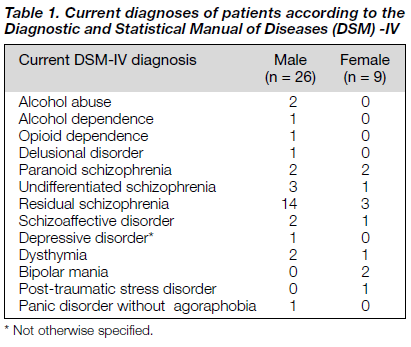
The Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I) gives a comprehensive profile of the Axis I disorders suffered by each patient currently and in his or her lifetime (Tables 1 and 2).8 Four male patients and two female patients suffered from current co-morbidity. The co-morbidity included alcohol and heroin dependence, alcohol abuse, and post- traumatic stress disorder. The mental health staff were not aware of the co-morbidity. Seven male patients and one female patient suffered from co-morbidity since the onset of mental illness. The co-morbidity included post-psychotic depression, cannabis abuse, and heroin abuse.
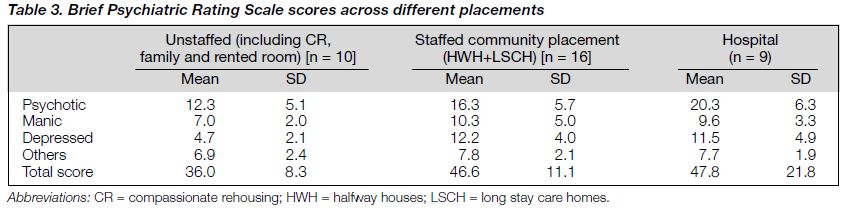
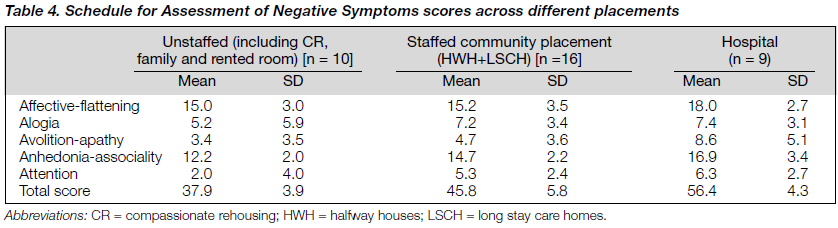
Table 3 shows the BPRS (Brief Psychiatric Rating Scale) ratings for the patients according to different placements. Using the Kruskal-Wallis test, there was no statistically significant difference for the BPRS scores across all three groups (p > 0.05). Table 4 shows the SANS (Schedule for Assessment of Negative Symptoms) scores across different placements. There was a statistically significant difference in negative symptoms in terms of volitional impairment (p = 0.05), social skills (p = 0.49) and attention (p = 0.50) across all three groups, using the Kruskal-Wallis test. Furthermore, the patients in the community had better grooming and hygiene, higher persistence at work or school and better physical energy when compared with hospitalised patients (p = 0.020, avolition score).
The total SANS score showed a statistically significant difference between that of in-patient and of out-patient status (p = 0.049). From the scores of BPRS and SANS, patients living at home had the lowest degree of psychopathology in terms of positive and negative symptoms (mean total BPRS = 36; mean total SANS = 37.9). The patients in hospital fared no worse than those in the community, in terms of positive symptoms. However, their negative symptoms, especially those of volition and apathy, distinguished them from outpatients.
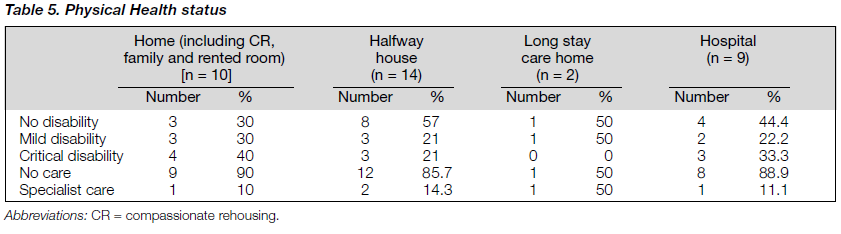
PHYSICAL HEALTH
Table 5 shows the level of disabilities and care needs across different settings. There were 10 patients with critical disabilities (tardive dyskinesia). However, none of the 10 patients had received any specific treatment for the tardive dyskinesia that was known to the care staff.
LIVING ENVIRONMENT AND DEGREE OF RESTRICTIVENESS
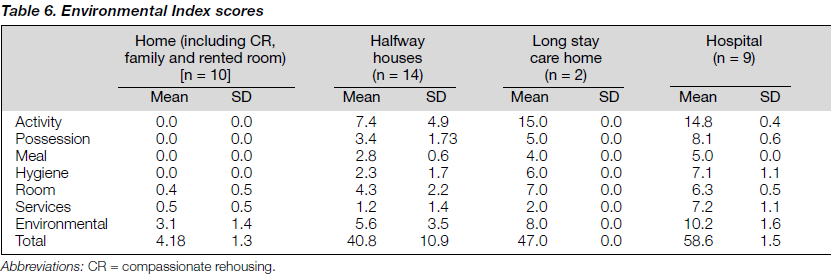
There was a marked difference between hospital and com- munity placement in terms of living conditions (in-patient 8.1, SD 3.7; out-patient 13.3, SD 3.5; mean difference 5.2; p = 0.003). There was also a statistically significant difference between patients living at home and those in supervised community settings (p = 0.012). The patients who lived at home tended to see their home as more attractive. The other scale of measurement about the degree of autonomy is the
Environmental Index.11 Table 6 shows the degree of freedom in these seven areas according to placement in the community and in hospital. All sub-scales were statistically significant across different community placements (p = 0.000). The patients in the community consistently enjoyed more freedom in the environment, in terms of jnlSubHeadlevel, meal preparation, self-care, budgeting, and personal privacy.
FORENSIC RECORDS AND POLICE INVOLVEMENT
Four patients had a history of violence with hospital order to a forensic unit. These offences were all committed before discharge from Castle Peak Hospital in 1993-1994. Five years after discharge to the community, only two patients were involved in inquiry by police for possible drug trafficking. Only two patients were fined. However, three patients reported having been attacked by others in the community.
WORK RECORDS AND WORK ADJUSTMENT IN THE COMMUNITY
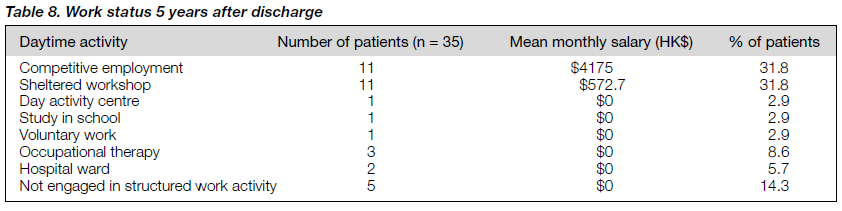
Table 7 shows the daytime activities of patients after discharge from Castle Peak Hospital to halfway houses. Table 8 shows the work status 5 years after discharge. The number of people actively working for a salary, be it in a sheltered workshop or competitive employment decreased from 85.7% to 63.6% in the 5 years after discharge to the community. 10 patients became unemployed after 5 years — the mean period of unemployment was 30 months).
On comparing the unemployed patients (n=13) with the rest of the sample, there was a statistical significance in avolition-apathy sub-score (p < 0.05), with unemployed patients having a significantly worse avolition-apathy sub- score. There were no other significant differences in BPRS total scores, sub-scores, or other SANS scores. On comparing those who remained competitively employed (n = 11) with the rest of the sample, those who remained in employment were more likely to remain in their initial jobs for a longer period of time (p < 0.005). There was no significant difference between those who were competitively employed from the remainder in terms of BPRS and SANS scores, duration of hospitalisation, and the number of jobs during the past 5 years. For patients working in a sheltered workshop 5 years previously, only 1 of 9 graduated from the sheltered workshop and became a sanitary worker.
SOCIAL NETWORK
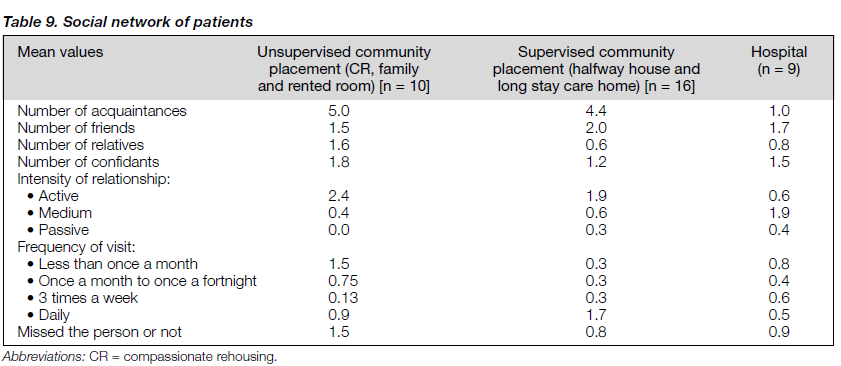
Table 9 shows the social network of the patients in the month before the interview. The mean number of friends of each patient was 1.8. The mean number of relatives was 0.8 and that of confidants was 1.3. There was no statistical difference in number of friends, relatives or confidants; frequency of visits by friends or relatives across different placements. However, the community group had a significantly higher number of acquaintances (p = 0.004), meaning that these patients had some integration into society. The community patients also had significantly more relationships of active intensity than that of hospitalised patients (p = 0.048).
SOCIAL ROLE FUNCTIONING IN THE COMMUNITY
Each patient had at least one disability in one of the eight role functions. 21.4% of patients in the community had mild disabilities in self-care compared with 88.7% of in-patients. Family role indicates the ability to function as a member in a family; all patients in supervised settings in the community or hospital had moderate to severe family role dysfunction. Kinship role indicates relationship with parents and siblings. All patients in hospital had moderate to severe disabilities. 48.6% of the sample were moderately or severely disabled in that role. Patients across all settings had disabilities in partner role function, which included functioning as a spouse or desire to have an intimate relationship. 24 of 35 patients (68.6%) had moderate to severe disabilities in partner role. Citizen role encompasses interest about news and the surrounding people and environment. 44.4% of hospitalised patients had moderate to severe disabilities. However, around 20% of patients in halfway houses and at home also had moderate to severe disabilities. Social role indicates ability to for m friendship. 34.3% of patients were moderately or severely disabled in that role. Occupational role indicates an ability to fulfil obligations in the daytime activity, be it housework or sheltered work. A high proportion of patients in a halfway house (71.5%) and in hospital (77.7%) were moderately to severely disabled in the occupational role. 23 of 35 patients (65.7%) had moderate to severe disabilities in an occupational role.
NEEDS ASSESSMENT BY USERS AND STAFF
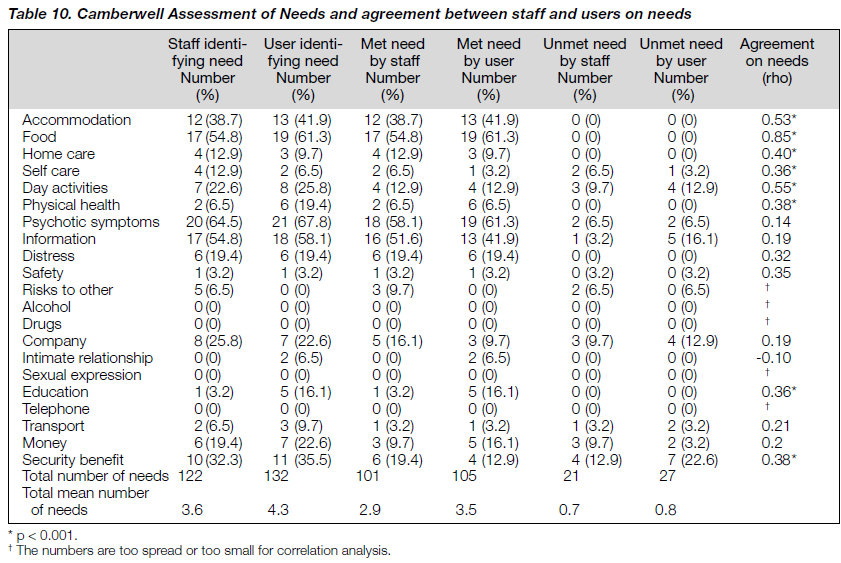
Table 10 shows the areas of need and the agreement between staff and users. There was no statistically significant difference between the mean numbers of needs (met and unmet) identified by users and carers (p = 0.212).
DISCUSSION
MENTAL HEALTH
The worst outcome for a patient is death. Four patients died during the 5-year follow-up. This represents 7.8% of the 51 dischar ged patients. All were men and suffered from schizophrenia, although all died of medical problems, not suicide or homicide. The mean age of the four patients was 43.2 years. The age-standardised mortality ratio of 40- to 44-year-old males in 1996 per 1000 was just 1.9.15
This was translated to only 0.1 in 51. The mortality rate in this sample was therefore much higher than expected. Brown demonstrated in a meta-analysis that patients with schizophrenia had increased mortality from natural and unnatural causes.16
The alcohol and heroin problems were not known to the health workers. This was in need of intervention in view of the evidence that failure to address co-morbid substance use disorders in mental disorders predicts a poorer outcome.17
Mental health workers should have a high index of suspicion for the possibility of substance misuse.
Patients living in the community had a mean BPRS score of 42.2, which was not statistically different from the mean BPRS score of 47.8 of hospital patients. Kane defined a BPRS score of over 45 as significantly severe psycho- pathology.18 Therefore, patients in both the community and hospital could be regarded as at least moderately psychotic. It was interesting that patients in both a halfway house and hospital were psychotic to more or less the same extent. What was the possible factor affecting discharge from halfway house and admission to hospital? The results of the negative symptom scores showed that the total SANS score and the ‘avolition-apathy’ sub-score appeared to distinguish between in-patient and out-patient status. The negative symptoms are known to be better predictors of psychosocial outcome in schizophrenia.19
PHYSICAL WELL BEING
The physical health of mentally ill patients is known to be worse than in the general population and medical co-morbidity is often under-recognised.20 In this study, 10 patients suffered from ‘critical disability’, namely tardive dyskinesia (TD). This represents a prevalence of 28.6% in this group of patients. Yassa and Jeste analysed 76 published studies and found a reported TD prevalence of 3% to 62% among treated patients with neurolepsy, with a mean of 24.4%.21 This figure is close to the reported prevalence in this sample. Another point of concern was the absence of any level of care for the problems as reported by the clinical staff in halfway houses or outpatient department. Another possible explanation was that care had been given for the TD problem but this information had not been clearly received and understood by the care staff in halfway houses or by the community psychiatric nurses. Both possibilities warrant further investigation and rectification.
QUALITY OF THE ENVIRONMENT
The study patients in the community rated their living environment and the degree of restrictiveness in the residence significantly better than those living in hospital (home, 4.2; halfway house, 40.8; long stay care home, 47.0; hospital, 58.6). In the TAPS study, the score for the community home was just below 10 while the score for the hospital was 26 of 55.22 The Environmental Index (EI) was slightly expanded in the subsequent TAPS study so that the total EI score was 60. The score reported here by Trieman referred to the use of the original EI where the total score was 55.23 There was a large difference in the degree of freedom found in TAPS in hospital practice in the UK compared to that in supervised settings in Hong Kong.
Shepherd compared a random sample of community residential homes with a sample of hospital rehabilitation wards.22 The basic provision of privacy and care of personal possessions was absent in hospital but the community homes were more homely in atmosphere. The author commented that the usual restrictions of hospital settings may result partly from their having to look after a very disabled group of residents, but might also be related to the training and attitudes of staff. The author argued that better training could result in an improved quality of life for patients in their care. The patients in hospital undoubtedly had severe positive and negative symptoms (mean total BPRS, 47.8; mean total SANS, 56.4). However, Shepherd’s argument may be valid in this situation.22
Although patients in the community perceived the degree of attractiveness and state of repair in community residence as better, the degree of restrictiveness still differed markedly between a home and halfway house. According to King et al. they differentiated ‘resident-oriented’ from ‘institutionally- oriented’ practices.24 Institutionally-oriented practices included block treatment of residents, rigidity of routines, and excessive social distance between staff and residents. Wing and Furlong argued that this was not confined to hospital settings but was also found in the community.25 The training needs of hostel workers needed to be addressed to reduce expressed emotion and institutionalised practices.26
Although patients living independently rated the living environment highest compared with other patients in supervised settings, the actual condition might still be below the normal standard compared with the general population. Mak and Gow found that patients discharged from halfway houses to the community were living in substandard con- ditions compared with their neighbours.27 In fact, this was also a point raised by Mak and Chan, about the use of the term ‘quality of life’ (QOL).29 They argued that when we did not know the average QOL of the general population, it was difficult to comment objectively about the QOL of the disadvantaged group.28
FORENSIC RECORD AND POLICE INVOLVEMENT
This group exhibited no violent behaviour to themselves or to others in this 5-year follow-up period. There was no sexual or physical violence. In fact, three patients had been victims of violence by others, two as victims of robbery and one as a victim of indecent assault. This finding supported the TAPS finding that the crime rate of discharged patients in the community was low and that patients were actually vulnerable in the community and needed protection from city violence.29
WORK RECORDS AND WORK ADJUSTMENT
In a recent study, it was found that employed individuals displayed less psychopathology and significant advantages in terms of subjective and objective measures of income and well being. Work was concluded to be associated with a better quality of life.30 In this study, only 10 patients were com- petitively employed and their mean monthly salary was only HK$4175. In 1996, the median monthly income of an elementary service worker was HK$5500.31 The unemployed patients, including those in a sheltered workshop, received a monthly benefit of HK$1799.32 Therefore, all patients had a lower income to support life compared with the general population.
In this study, the patients showed a significant increase in the number becoming unemployed. Twenty-one patients worked at discharge, while only 11 patients remained at work after 5 years. The remaining 10 patients became unemployed. This agrees with the finding of Lai, et al. that, after living in a halfway house for a year, there was a significant increase in unemployment.33
Because the study was performed in 1998, it might be speculated that the high unemployment rate in the sample was due to the economic recession in Hong Kong. However, the mean period of unemployment was 30.0 months, and occurred well before the onset of the economic recession. The reasons quoted for losing a job were firing by boss or quitting by self, suggesting work performance or work-related interpersonal skills deficit. This might be partly explained by the finding of more severe avolition-apathy sub-score in the unemployed group. Bond argued that few resources had been directed to the post-placement period resulting in a disappointing rate of job retention and that the priorities on work training must be re-evaluated.34
In the sample, only 11.1% of those in a sheltered workshop ‘graduated’ after 5 years. This was contrasted with the finding in the Western literature that 10% of workshop clients were placed in competitive employment annually (information from Greenleigh Associates, 1975, quoted by Bond34). Mak found that sheltered workshops failed to reveal any significant factors within the workshops that could contribute to successful open employment of the workers in the community.35 The sheltered workshop training and management practices in Hong Kong were criticised by a local author.36 Supported employment is now beginning in Hong Kong.37 This approach of vocational rehabilitation awaits further evaluation to see if it helps more severely mentally ill clients to obtain competitive employment.34
SOCIAL NETWORK
In the study group, the mean number of friends and relatives of each patient was 1.8 and 0.8, respectively. The mean number of confidants was only 1.3. The number of acquain- tances was higher in the community group, meaning better integration into the local community. However, the mean total network size was 7.8. There was no data in this study to compare with ordinary people in Hong Kong. However, in the TAPS study, the baseline total network size for each chronically-ill patient was 8, which was regarded as small according to British standards.29 Furthermore, this has to be evaluated against the Chinese culture, which places much importance in interpersonal relationships in every day social lives of Chinese. Traditional and contemporary Chinese place strong reliance on interpersonal bases for defining social status.38 Chinese people might be more likely to have an even wider social network than their counterparts in the West.
SOCIAL ROLE IN SOCIETY
The importance of social role functioning in Chinese society was highlighted by Yang,38 who argued that Chinese culture was a relation-based one and Chinese people had strong relationship-orientation. This might support social role functioning assessment as an important dimension in quality of life study. A Chinese person without a role as a family member is likely to suffer low self-esteem and attract more criticism from others when compared with a Wester n counterpart. In this sample, all patients had at least one disability in any of the eight role functions. It was apparent that a substantial number of the sample here had major disabilities in family, kinship, and occupational roles. As most of the patients were living in supervised settings (25 of 35 patients), the disability in family role was understandable as they were unable to fulfil expectations as a usual family member. The patients were discharged from Castle Peak Hospital to halfway houses, indicating that most had difficulty in re-integrating back to his or her family. However, after 5 years in the community, only 18 of 35 patients had no or mild disabilities in the kinship role. It was worth noting that lack of opportunities of interaction with parents was not considered as a disability in the Groningen Scale.39 Therefore, the disabilities refer to the actual kinship relationship after the duration, frequency, and other exter nal constraints have been taken into consideration. Schene et al. found that more than 50% of family carers had ‘burn-out’ and 60 to 90% felt desperate about caring for a chronically-ill mental patient.40 Therefore, it is not surprising that many patients still had difficulty in their relationship with family members. Perhaps family intervention might be of help for relatives coping with the problems of living with a person with schizophrenia.41
WHAT ARE THEIR NEEDS?
The CAN showed that the mean number of needs perceived by patients was 4.3 and the mean numbers of met and unmet needs were 3.5 and 0.8, respectively. The mean number of needs perceived by staff was 3.6. There was no significant difference in the number of needs perceived by patients themselves and the staff. In another study, the difference of needs was of statistical significance.42
In some domains such as alcohol and drugs, there was no need as perceived by both patients and staff. This must be contemplated against the objective finding in SCID that four patients were current substance abusers. Furthermore, the agreement between the staff and patients on the presence of need was only statistically significant in domains of material need like food and accommodation. However, the agreement was not high even in these domains (0.36-0.55) except in the domain of ‘food’. No patients rated having intimate relationship and sexual expression need. In Slade’s study, 28% of patients rated having intimate relationship need and 10% ratted having sexual expression needs.42
The low number of private needs must be evaluated against the high level of social role disabilities. This sample was a group of relatively chronically-ill patients. Long-term psy- chiatric patients have suffered severe role constrictions in their lives as a result of disabling mental problems or of having spent large portions of their life in psychiatric institutions. Low aspirations and depressed level of expectations might lead individuals to report satisfaction with life conditions that are considered inadequate by healthy people.43 Furthermore, this group had a mean total SANS score of 46.3, representing a moderate to severe degree of negative symptoms. This might explain why they had a reduced need for company, sexual expression, and intimate relationship. Poverty of speech and impoverished thinking might have affected the response to a structured interview such as CAN.
Furthermore, Chinese culture of relational fatalism, believing in fatalistic factor, or yuan, in determining occur-rence, type, duration, and final outcome of an interpersonal relationship led to an attitude of passive acceptance of a relationship.38
Patients might feel resigned that no one could help even if such need for intimate relationship was expressed. Chinese also show much polite and respectful restraint when faced with authority figures.38 It would be extremely difficult to express personal needs in front of an authority figure such as a mental health professional. This might explain the lower number of needs in all domains, especially highly personal ones.
CONCLUSIONS
Patients enjoyed autonomy and freedom in the community. However, many patients had sub-standard quality of life after re-settlement in the community. They had very restricted social roles, small social networks, and unstructured daily lives. Physical, psychiatric and drug problems went undetected. Community re-settlement is highly treasured by the patients, but comprehensive and adequate support in the community is essential to make it a success.
LIMITATIONS OF THE STUDY
The study population was a group of chronic psychotic patients with a long history of psychiatric problems and admission records. They were different from the general psychiatric population in that they were all psychotic with severe psychopathology. They also had a very poor social support network before dischar ge from Castle Peak Hospital. Therefore, they could not be representative of the general psychiatric population.
The study had a small sample size restricted to a single psychiatric unit, thus reducing the power and representative- ness of the study. A multi-centre collaborative study may provide a more comprehensive picture of the discharged patients in the community. This is only a retrospective study so the issue of benefits of community re-settlement is not addressed. A prospective study or a case-control study will shed more light into this crucial question. It must be noted that 25% of the sample was not interviewed, so their quality of life was not known.
REFERENCES
- Campell A. Subjective measures of well-being. Am J Psychol 1976; 15:117-124.
- Albrecht GL, Fitzpatrick R. A sociological perspective on health-related quality of life research. Advances in Medical Psychology. Vol 5. Quality of Life in Health Care. London: London; 1994.
- Katschnig H. How useful is the concept of quality of life in psychiatry? In: Katschnig H, Freeman H, Sartorius N (editors). Quality of life in mental disorders. Chichester: John Wiley & Sons; 1997:3-16.
- Becker M, Diamond R, Sainfort F. A new patient focused index for measuring quality of life in persons with severe and persistent mental illness. Qual Life Res 1993;2:239-251.
- Barry MM, Crosby C. Quality of life as an evaluative measure in assessing the impact of community care on people with long-term psychiatric disorders. Br J Psych 1996;168:210-216.
- Kay D, Beamisch P, Roth M. Old age mental disorders in Newcastle- upon-Tyne, II. A study of possible social and medical causes. Br J Psych 1964;110:668-682.
- Castle Peak Hospital. Annual Report: 1996-1997.
- 8. First MB, Spitzer RL, Gibbon M, Williams JBW. Structured Clinical Interview for DSM-IV axis I disorders. Washington: American Psychiatric Press;
- Lukoff D, Liberman RP, Nuechterlein KH. Symptom monitoring in the rehabilitation of schizophrenic patients. Schizophr Bull 1986;12:578-602.
- Andreasen NC. The scale for the assessment of negative symptoms (SANS). University of Iowa: Iowa; 1983.
- O’Driscoll C, Leff J. The TAPS project. 8: design of the research study on the long-stay patients. Br J Psych 1993;162 (Suppl.19): 18-24.
- Leff J, O’ Driscoll C, Dayson D, Willis W, Anderson J. The TAPS project. 5: The structure of social network data obtained from long-stay patients. Brit J Psych 1990;157:848-852.
- Wiersma D, De Jong A, Kraaijkamp HJM, Ormel J. GSDS-II. The Groningen social disabilities schedule, second version. Manual, questionnaire and rating form. Department of Social Psychiatry: University of Groningen; 1990.
- Phelan M, Slade M, Thornicroft G, et al. The Camberwell assessment of need: the validity and reliability of an instrument to assess the needs of people with severe mental illness. Br J Psych 1995;167:589-595.
- Census and Statistics Department. Demographic trends in Hong Kong 1981-1996. Hong Kong: Printing Department of Hong Kong Special Administrative Region Government;1997:41.
- Brown S. Review: patients who have schizophrenia have increased mortality from all causes, natural causes, and unnatural causes. Evidence-Based Mental Health 1997;3:91.
- Helzer JE, Psyzbeck TR. The co-occurrence of alcoholism and other psychiatric disorders in the general population and its impact on treatment. J Stud Alcohol 1988;49:219-224.
- Kane J, Honigfeld G, Singer J, Meltzer HY, the Clozapine Collaborative Group. Clozapine for the treatment-resistant schizophrenic: a double-blind comparison with chlorpromazine. Arch Gen Psych 1988;45:789-796.
- Andreasen NC, Roy MA, Flaum M. Positive and negative symptoms. In Hirsch SR, Weinberger DR (editors). Schizophrenia. London: Blackwell;1997:28-45.
- Jeste DV, Gladsjo JK, Lindamer LA, Lacro JP. Medical co-morbidity in schizophrenia. Schizophr Bull 1996;22:413-430.
- Yassa R, Jeste DV. Gender differences in tardive dyskinesia; a critical review of the literature. Schizophr Bull 1992;18:701-715.
- Shepherd G, Muijen M, Dean R, Cooney M. Residential care in hospital and in the community — quality of care and quality of life. Br J Psych 1996;168:448-456.
- Trieman N. Residential care for the mentally ill in the community. In Leff J (Editor). Care in the Community, Illusion or Reality? Chichester: Wiley;1997:51-68.
- King RD, Raynes NV, Tizard J. Patterns of residential care. London: Routledge & Kegan Paul: 1971.
- Wing JK, Furlong R. A haven for the severely disabled within the context of a comprehensive psychiatric community service. Br J Psych 1986;149:449-457.
- Lavender A, Sperlinger A. Staff training. In Lavender A, Holloway F (Editors). Community care in practice. New York: Wiley; 1988: 149-158.
- 27. Mak KY, Gow L. The living conditions of psychiatric patients discharged from halfway houses in Hong Kong. Int J Soc Psychiatry 1991;37:107-112.
- Mak KY, Chan KKC. The quality of life issue in psychiatry. HK J Mental Health 1990;19:37-41.
- Leff J. The outcome of long-stay non-demented patients. In: Leff J (Editor). Care in the community: illusion or reality? Chichester: Wiley; 1997:69-92.
- Priebe S, Warner R, Hubschmid T, Eckle I. Employment, attitudes toward work, and quality of life among people with schizophrenia in three countries. Schizophr Bull 1998;24:469-477.
- Census and Statistics Department. 1996 Population by census. Hong Kong: Government Printer;1996:96.
- Director of Social Welfare. 1996-1997 Departmental Hong Kong: Government Printer;1997:13.
- Lai B, Li EWF, So AWK. A follow-up study of social adjustment of halfway house residents. I: Outcome of social adjustment in one year. HK J Mental Health 1988;17:67-73.
- Bond G. Vocational rehabilitation. In: Liberman RP (Editor). Handbook of psychiatric rehabilitation. Massachusetts: Simon & Schuster;1992:244-270.
- Mak KY, Wong D. Supported employment: a breakthrough in vocational rehabilitation. HK J Mental Health 1993;22:37-42.
- Ng PYN. The problems of sheltered workshop for the mentally ill in Hong Kong. HK J Mental Health 1993;22:76-84.
- Mak KY, Wong D, Lee A, Wong FK, Tsang F, Chung PK. An exploratory study on sheltered employment of psychiatrically disabled persons in Hong Kong. The HK Council of Social Services; 1993.
- Yang KS. Chinese social orientation: an integrative analysis. In: Tsung YL, Tseng WS, Yeh EK (Editors). Chinese societies and mental health. New York: Oxford;1995:19-39.
- Wiersma D. Role functioning as a component of quality of life in mental disorders. In Katschnig H, Freeman H, Sartorius N, editors. Quality of life in mental disorders. Chichester: Wiley;1997: 32-42.
- Schene AH, Tessler RC, Gamache MG. Instruments measuring family or caregiver burden in severe mental illness. In: Thornicroft G, Tansella M (Editors). Mental health outcome measures. Berlin: Springer-Verlag;1996:53-73.
- Leff J. Needs of the families of people with schizophrenia. Adv Psych Treatment 1998;4:277-284.
- Slade M, Phelan M, Thornicroft G. A comparison of needs assessed by staff and by an epidemiologically representative sample of patients with psychosis. Psychol Med 1998;28:543-550.
- Barry MM. Well-being and life satisfaction as components of quality of life in mental disorders. In: Katschnig H, Freeman H, Sartorius N (Editors). Quality of life in mental disorders. Chichester: John Wiley & Sons Ltd;1997:20-30.
Acknowledgement: This study was supported partly by a fund raised by the second author. We would like to thank the two nurses, Mr Karl Ng and Miss Florence Kan and the three occupational therapists, Miss Ada Lo, Mr Godwin Tai, and Miss Vannes Wong, for participating in the study. We would also like to thank the ward manager of the hospital pre-discharge unit, Miss YW Pang, for her efforts in tracing the patients.
Dr RMK Ng, MBchB, MRCPsych, FHKAM (Psychiatry), Senior Medical Officer, Hospital Pre-discharge Unit, Castle Peak Hospital, Hong Kong, China.
Dr SP Leung, MBBS, MRCPsych, FHKAM (Psychiatry), Chief of Service, Castle Peak Hospital, Hong Kong, China.
Address for correspondence: Dr Roger Ng
Senior Medical Officer
Castle Peak Hospital,
15, Tsing Chung Koon Road,
Tuen Mun,
Hong Kong, China.