East Asian Arch Psychiatry 2013;23:21-8
REVIEW ARTICLE
Dr Jegan Yogaratnam, MBBS, MD, Institute of Mental Health / Woodbridge Hospital, Singapore.
Dr Neetesh Biswas, MBBS, Institute of Mental Health / Woodbridge Hospital, Singapore.
Dr Ramyadarshni Vadivel, MBBS, Institute of Mental Health / Woodbridge Hospital, Singapore.
Dr Rajesh Jacob, MBBS, MD, Institute of Mental Health / Woodbridge Hospital, Singapore.
Address for correspondence: Dr Jegan Yogaratnam, Woodbridge Hospital / Institute of Mental Health, 10 Buangkok View, Singapore 539747.
Tel: (65) 6389 2000; Fax: (65) 6385 5900; email: jegany@gmail.com
Submitted: 25 June 2012; Accepted: 10 September 2012
Metabolic syndrome is a cluster of risk factors comprising obesity, dyslipidaemias, glucose intolerance, insulin resistance (or hyperinsulinaemia), and hypertension, and is highly predictive of type 2 diabetes mellitus and cardiovascular disease. The life expectancy of people with schizophrenia is reduced by 20%, with 60% of the excess mortality due to physical illness. Schizophrenia itself may be a risk factor for metabolic syndrome and there is also increasing concern that antipsychotic drugs, particularly second- generation antipsychotics, have metabolic consequences that contribute to the risk. Various diagnostic guidelines, updated facts with regard to epidemiology, pathophysiology, risk factors, and complications of metabolic syndrome are discussed in this review. Moreover, the impact of various antipsychotics on metabolic syndrome and their possible mechanisms are comprehensively reviewed. The authors emphasise that, while many adults with schizophrenia receive little or no medical care, such care is important given the risk of metabolic abnormalities associated not only with antipsychotic medications, but also with schizophrenia in general.
Key words: Antipsychotic agents; Metabolic syndrome X; Metabolism; Schizophrenia
摘要
代谢综合症是肥胖、血脂异常、葡萄糖耐受不良、胰岛素抗性(或称高胰岛素血症)和高血压 等的风险因素群,并且能高度预测二型糖尿病和心血管疾病。精神分裂症患者的寿命一般缩短 20%,而因身体疾病导致的额外死亡率也达到60%。精神分裂症本身也许是代谢综合症的风险 因素,而抗精神病药,尤其是第二代抗精神病药对代谢功能的影响也渐受关注。本文回顾并讨 论代谢综合症各种诊断指南以及有关其流行病学、病理生理学以及风险因素和併发症的最新资 讯。本文也回顾各种抗精神病药对代谢综合症的影响和其可能机制。代谢异常的风险不仅与抗 精神病药,且与精神分裂症相关。因此,在现行对成人精神分裂症患者相关护理不足甚至缺乏 的情况下,作者强调它的重要性。
关键词:抗精神病药、代谢综合症、代谢、精神分裂症
Metabolic syndrome is a cluster of risk factors comprising obesity (central and abdominal), dyslipidaemias, glucose intolerance, insulin resistance (or hyperinsulinaemia), and hypertension, and is highly predictive of type 2 diabetes mellitus and cardiovascular disease.1 The mean age of death is 61 years for patients with schizophrenia, which is considerably younger than 76 years for the general population.2 Life expectancy in people with schizophrenia is reduced by 20%,3 with 60% of the excess mortality due to physical illness.4
Schizophrenia itself may be a risk factor for metabolic syndrome in addition to many other factors in patients with schizophrenia, and there is also increasing concern that antipsychotic drugs, particularly second-generation antipsychotics (SGAs), have metabolic consequences that contribute to the risk.5 The precise relationship between antipsychotic drugs and metabolic syndrome remains uncertain, but it is clear that people with schizophrenia treated with antipsychotic medications develop individual features of metabolic syndrome, and the syndrome itself, at a higher rate than the general population. Antipsychotic polypharmacy, which is a common practice in many psychiatric settings, as compared with monotherapy, may be independently associated with increased risk of pre-metabolic syndrome and higher rates of metabolic syndrome and lipid markers of insulin resistance, even after adjusting for patients’ lifestyle characteristics.6,7 A recent study concluded that switching to monotherapy was appropriate and reasonable as long as patients could return to polypharmacy when necessary, and switching from a higher- to a lower-risk agent or from polypharmacy to monotherapy may facilitate metabolic improvement.8
Many reviews have concluded that there is a need for active routine physical health screening of all individuals receiving treatment with antipsychotic drugs,9 which is in keeping with the recommendations of the National Institute for Health and Clinical Excellence treatment guidelines for schizophrenia. While many adults with schizophrenia receive little or no medical care, such care is important, given the risk of metabolic abnormalities associated not only with antipsychotic medications, but also with schizophrenia in general.10
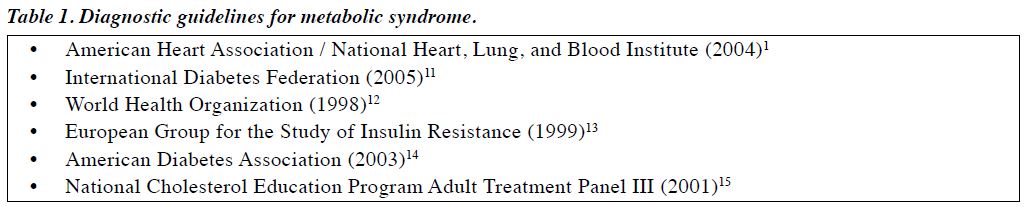
Guidelines for diagnosis of metabolic syndrome are listed in Table 1.1,11-15 The most commonly used definitions for metabolic syndrome are in keeping with the Adult Treatment Panel III (ATP III) of the National Cholesterol Education Program (NCEP) definition and the adapted ATP III recommendation proposed by the American Heart Association which follows the International Diabetes Federation (IDF) guideline of lowering the threshold for impaired fasting glucose to 5.56 mmol/L (100 mg/dL).11 An important difference between the NCEP / ATP III and the IDF definitions is that of the values for central obesity, which are defined as > 102 cm for men and > 88 cm for women in the NCEP / ATP III definition, the IDF values are comparatively lower at 94 cm and 80 cm, respectively, with a lower value of 80 cm for South-Asian men.16
Metabolic syndrome is a burgeoning global problem, with approximately 25% of adult Europeans and Latin Americans, 22% of US adults, and 32% of Mexican Americans17 estimated to have the condition. Additionally, metabolic syndrome is considered an emerging epidemic in developing East-Asian countries, including China, Japan, and Korea, where the prevalence ranged from 8 to 13% in men and 2 to 18% in women depending on the population and definitions used.18 Even in many other countries worldwide, metabolic syndrome has been recognised as a highly prevalent health problem19 demanding attention and intervention. The exact prevalence of metabolic syndrome in patients with schizophrenia is unknown. Using baseline data from the Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) schizophrenia trial, the prevalence of metabolic syndrome was 40.9% and 42.7% according to the NCEP and the American Heart Association / National Heart, Lung, and Blood Institute–derived criteria, respectively.20
Metabolic syndrome is thought to be caused by adipose tissue dysfunction and insulin resistance. Dysfunctional adipose tissue results in the release of proinflammatory cytokines such as tumour necrosis factor, adiponectin, leptin, resistin, and plasminogen activator inhibitor, which play an important role in the pathogenesis of obesity-related insulin resistance, the primary mediator of metabolic syndrome.21
People with schizophrenia on average have a sedentary lifestyle involving lack of regular physical activity, poor food intake, substance abuse, and high rates of smoking,22 which increase their risk for development of metabolic syndrome in addition to the risk from antipsychotic medications. These lifestyle factors are partly influenced by aspects of the illness such as negative symptoms and vulnerability to stress. Moreover, earlier studies have shown an increased risk for people with schizophrenia to develop metabolic abnormalities in the absence of antipsychotic medication, and there are indications of an increased risk for diabetes in first-degree relatives of patients with schizophrenia.23
Other possibilities to explain these associations in schizophrenia include stress and abnormalities of the hypothalamic-pituitary-adrenal axis.24 A study showed that people with schizoaffective disorder are more vulnerable to metabolic syndrome than people with schizophrenia for unexplained reasons.25
The complications of metabolic syndrome are broad. Table 226-30 shows that metabolic syndrome is a multisystem disorder involving the cardiovascular, hepatobiliary, and central nervous / psychological systems.
Notwithstanding the therapeutic effectiveness of antipsychotic drugs in many illnesses such as schizophrenia, increased attention has turned to the possible deleterious side-effects of these agents. Metabolic derangements associated with antipsychotic agents have been the focus of considerable interest and debate for many years. While metabolic syndrome affects all ages of patients who take antipsychotic medications, children and adolescents receiving atypical antipsychotic medications are particularly vulnerable to these effects.31 Notably, obesity-associated metabolic disease short of type 2 diabetes mellitus (i.e. dyslipidaemia and hypertension in the absence of type 2 diabetes mellitus) may be mechanistically linked to lower academic and professional potential in adolescents, as lower cognitive performance and reduction in brain structural integrity among adolescents with metabolic syndrome has been documented in studies.32
While there appears to be a dose-dependent relationship between the dose of clozapine or olanzapine and metabolic complications, aripiprazole, quetiapine, and ziprasidone do not show a causal relationship, and risperidone has mixed results.33
Interestingly, an independent association between schizophrenia and physical illnesses that have a metabolic signature, including obesity, has been proposed, with several studies reporting significantly higher (p < 0.001) prevalences of overweight (body mass index [BMI] ≥ 25 kg/m2) and obesity (BMI > 30 kg/m2) in patients with psychotic disorders than in the general population.34 Drug- naïve schizophrenia patients have also been found to have more than 3 times as much intra-abdominal fat (which is correlated with insulin resistance) as age- and BMI- matched control participants,35 supporting the independent association between psychosis and weight gain. Additionally, weight gain typically occurs within the first 4 to 12 weeks of treatment and may not reach a plateau.36
While the prevalence of obesity in the medicated schizophrenic population is currently estimated to range from 40 to 60% versus 30% of the general adult population, the differences between typical and atypical agents with regard to the risk for weight gain and disorders of carbohydrate and lipid metabolism remain unclear, although weight gain and carbohydrate and lipid metabolism disorders may be more common in patients taking atypical agents.9 Several studies have supported the claim that treatment with atypical antipsychotics was associated with more weight gain than treatment with typical antipsychotics.37,38
Of the typical antipsychotics, lower potency agents (chlorpromazine and thioridazine) induce greater weight gain than higher potency drugs (fluphenazine and haloperidol). Typical antipsychotic-associated weight gain appears to be comparable for oral and depot formulations of the same drug.39 Of those atypical antipsychotics (SGAs), clozapine and olanzapine appear to have the greatest propensity to induce weight gain, quetiapine and risperidone have intermediate risk, followed by aripiprazole, ziprasidone, and amisulpride which carry the least risk (Table 338). Weight gain associated with risperidone and quetiapine does appear to correlate with dose, and newer antipsychotics such as bifeprunox, asenapine, iloperidone, and paliperidone are known to cause low weight gain.40
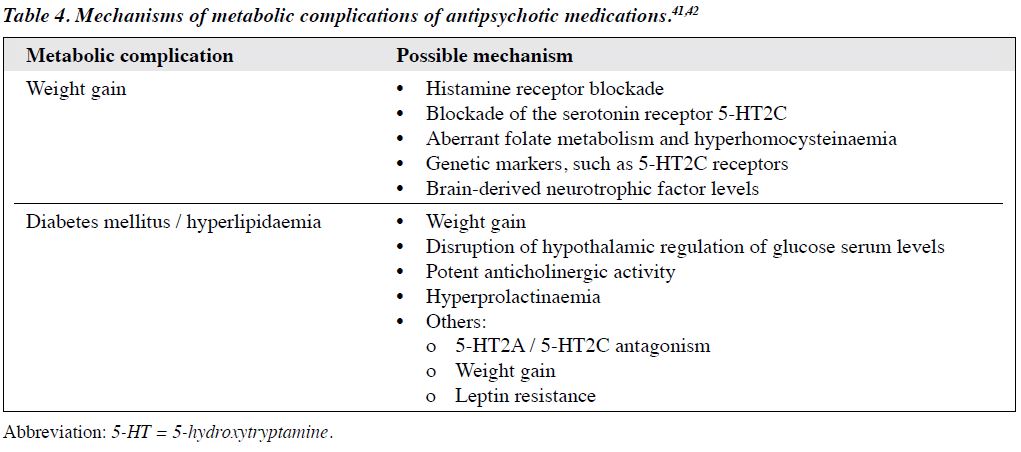
The mechanism of antipsychotic-induced weight gain is undetermined, but several neurotransmitter systems have been implicated (Table 441,42). Olanzapine, which has the highest affinity for histaminic receptors, is associated with high rates of weight gain, while ziprasidone and aripiprazole, with lower affinities for histamine receptors, are associated with lower rates of weight gain. A genetic predisposition for aberrant folate metabolism and hyperhomocysteinaemia and genetic markers, such as 5-hydroxytryptamine (5-HT) 2C receptor and brain-derived neurotrophic factor, and blockade of the serotonin receptor 5-HT2C have also been linked to risk for weight gain.43
Additional studies have found the prevalence of both diabetes and obesity to be 2 to 4 times higher in people with schizophrenia than in the general population, with overall prevalence estimates for diabetes among patients with schizophrenia ranging from 16 to 25%.44 Poor outcomes for diabetes in patients with schizophrenia are due to the reasons that their high rates of smoking (up to 75%) worsens the prognosis of diabetes and increases non- adherence to treatment for diabetes, which is estimated to be about 50%.45 Most cases of new-onset type 2 diabetes caused by antipsychotic medications occur within the first 6 months of treatment and are often, although not always, associated with significant weight gain or obesity. A family history of diabetes is also associated with an increased risk in this population.46
A large population-based case-control study found the risk of diabetes associated with antipsychotic agents to be quite variable.46 Olanzapine and risperidone had 4.2 and 1.6 times the risk associated with conventional agents, and 5.8 and 2.2 times the risk associated with no treatment, respectively. Several large retrospective population studies have found that olanzapine and clozapine are associated with a significantly higher rate of diabetes than the other agents, with a particular risk for younger patients.47 Quetiapine appears to be more likely than conventional drugs to be associated with diabetes, but may ameliorate clozapine-related diabetes when given in conjunction with clozapine.48 Data for aripiprazole and ziprasidone suggested that neither drug alters glucose homeostasis. Aripiprazole may even reverse diabetes caused by other drugs, although ketoacidosis has been reported with aripiprazole.49Among the traditional neuroleptics, chlorpromazine and thioridazine50 are the agents most closely associated with diabetes mellitus, although the associations are weaker than those with olanzapine or clozapine. The prevalence of impaired glucose tolerance seems to be higher with aliphatic phenothiazines than with fluphenazine or haloperidol, although haloperidol has been reported to increase insulin resistance and to be associated with higher fasting glucose levels in obese women compared with control participants.51
Interestingly, some studies have suggested that first- generation antipsychotics are no different from SGAs in their propensity to cause diabetes, whereas others have suggested a modest, but statistically significant excess incidence of diabetes with SGAs.52
A number of mechanisms for antipsychotic medication–induced diabetes mellitus have been suggested, although none has been proven with certainty (Table 441,42). While drug-induced weight gain has been highly associated with diabetes, diabetes has occurred in the absence of weight gain, and hypothalamic dopamine antagonism by antipsychotic medications or disruption of hypothalamic regulation of glucose serum levels have been suggested, along with potent anticholinergic-induced inhibition of insulin secretion.53 Other mechanisms suggested include increased insulin resistance in peripheral tissues caused by hyperprolactinaemia, 5-HT2A / 5-HT2C antagonism, increased lipids, weight gain, and leptin resistance.54
Phenothiazines are known to be associated with increased levels of triglycerides and low-density lipoprotein cholesterol and a decreased level of high-density lipoprotein cholesterol.55 Higher cholesterol levels have been reported with chlorpromazine-treated patients than those receiving haloperidol.56 The CATIE study showed that of the atypical antipsychotic agents, olanzapine and quetiapine are associated with increases in total cholesterol levels and triglyceride levels.56 Notably, risperidone and ziprasidone are associated with decreases in cholesterol and triglyceride levels, and patients treated with clozapine have triglyceride levels that are almost double those treated with typical antipsychotic agents.57 Aripiprazole and ziprasidone have minimal adverse effects on blood lipids and may even reverse dyslipidaemias associated with previous antipsychotic use.58
Although the exact mechanism of causation of hyperlipidaemia is unknown, one or more of the mechanisms described above as causes for antipsychotic medication– induced diabetes mellitus (Table 338) may be involved in the pathogenesis.
Although most of the emphasis on metabolic syndrome is aimed at SGAs, several studies have failed to detect differences in the prevalences of metabolic syndrome between patients taking SGAs and those taking conventional antipsychotic agents.59 It may be possible that the effects of conventional antipsychotic agents on metabolic symptoms have been underestimated. Support for this possibility comes from a study that compared olanzapine and haloperidol in patients with first-episode psychosis — a group of patients who were comparatively free of previous treatment and symptom chronicity.60 After 2 years, patients taking olanzapine had gained a mean of 33.9 lb (15.4 kg), and those taking haloperidol had gained 16.5 lb (7.5 kg) —a considerable weight gain indicating that typical antipsychotic agents are associated with weight gain and related metabolic abnormalities. A recent systematic review compared the metabolic effects among the different SGAs and showed that clozapine and olanzapine had the highest incidences.61
The following strategies have been suggested for directly caused adverse effects of antipsychotic agents on glucose– insulin homeostasis and lipid metabolism:
- Patients with previously diagnosed diabetes mellitus and / or hyperlipidaemia should be given conventional antipsychotic agents or atypical agents such as aripiprazole, which have no or few effects on glucose- insulin homeostasis and lipid metabolism.62
- For patients who develop hyperinsulinaemia and / or hyperlipidaemia during treatment with clozapine, olanzapine, or structurally related agents, a change to an antipsychotic drug with no or minimal capability to induce such adverse metabolic effects should be considered, or maintenance therapy with the lowest effective dose possible, together with regular follow- up of metabolic parameters and appropriate treatment whenever necessary, is advised.62
- For patients who develop diabetes mellitus during therapy with antipsychotic agents, a change to an antipsychotic agent with no or little propensity to cause the condition is the first recommendation. For patients taking clozapine, the lowest effective dose possible should be given, with clinical evaluation and determination of serum antipsychotic concentration, along with concomitant therapy for hyperlipidaemia / hyperglycaemia.62
- All patients who are going to start treatment with, or are already using an antipsychotic drug with high or intermediate propensity to induce weight gain should undergo regular monitoring of weight and lifestyle modifications / therapy such as dietary adjustments, weight reduction, and physical training, if necessary.
- If such a patient gains a considerable amount of weight or has become overweight or obese already, a change of the antipsychotic agent to a less weight-inducing drug should be considered. Another possibility to decrease antipsychotic-induced weight gain may be dose reduction. In the general population, controlled clinical trials have established modest efficacy for obesity drugs in combination with lifestyle therapy.63 Orlistat (a lipase inhibitor) and sibutramine (a serotonin-dopamine-norepinephrine reuptake inhibitor) are the only drugs currently approved for long-term weight loss.
- Interventions to stop cigarette smoking and to reduce physical inactivity are also of great importance in decreasing the risk of insulin resistance and type 2 diabetes mellitus in patients treated with antipsychotic agents.63
- In order to further decrease the risk for development of insulin resistance and type 2 diabetes mellitus in antipsychotic medication–treated patients, daytime sedation caused by these drugs, leading to physical inactivity, has to be recognised and handled properly.63
- Psychiatrists also have to be aware of those antipsychotic medication–treated patients who are older, have a family history of type 2 diabetes mellitus, and / or are of an ethnic group with high genetic susceptibility to type 2 diabetes mellitus (e.g. American Indians, Mexican Americans, and Hispanics) and, therefore, have an increased risk of developing insulin resistance and type 2 diabetes mellitus.63
In view of the evidence for an increased prevalence of metabolic syndrome in schizophrenia, individuals presenting with a first episode of psychosis should be screened using the appropriate diagnostic criteria.15 According to the Maudsley guidelines,40 metabolic parameters should be measured with the frequency as described below:
- Plasma glucose (fasting blood sample, if possible) should be done at baseline, at 4 to 6 months, and then yearly. Ideally, all patients should have oral glucose tolerance tests performed as this is the most sensitive method of detection of diabetes mellitus. Fasting plasma glucose tests are less sensitive but are still recommended.
- Blood pressure should be measured at the baseline and frequently during dose titration.
- Fasting blood lipids (cholesterol and triglycerides) should be measured at baseline, at 3 months, and then yearly. Patients prescribed clozapine, olanzapine, quetiapine, or phenothiazines should ideally have their serum lipids measured every 3 months for the first year of treatment.
- Weight (including waist circumference and BMI, if possible) should be measured at baseline, frequently for 3 months, and then yearly.
In summary, while many adults with schizophrenia receive little or no medical care, such care is important given the risk of metabolic abnormalities and metabolic syndrome associated with schizophrenia and with the antipsychotic medications used to treat the condition. There is a need for active routine physical health screening of all individuals receiving treatment with antipsychotic drugs. The implementation of such guidelines can substantially improve the health of patients with schizophrenia. However, adopting the guidelines in clinical practice can be challenging.
- Grundy SM, Brewer HB Jr, Cleeman JI, Smith SC Jr, Lenfant C; American Heart Association; National Heart, Lung, and Blood Institute. Definition of metabolic syndrome: Report of the National Heart, Lung, and Blood Institute / American Heart Association conference on scientific issues related to definition. Circulation 2004;109:433-8.
- Newman SC, Bland RC. Mortality in a cohort of patients with schizophrenia: a record linkage study. Can J Psychiatry 1991;36:239-45.
- Mazi-Kotwal N, Upadhyay B. Physical health in schizophrenia. Cutting Edge Psychiatry in Practice 2011;1:74-7.
- Barnes TR, Kerwin R. Mortality and sudden death in schizophrenia. In: Camm J, editor. Cardiovascular risk associated with schizophrenia and its treatment. London: Galliard Healthcare Communications; 2003: 7-23.
- Haddad PM. Antipsychotics and diabetes: review of non-prospective data. Br J Psychiatry Suppl 2004;47:S80-6.
- Reynolds GP, Kirk SL. Metabolic side effects of antipsychotic drug treatment — pharmacological mechanisms. Pharmacol Ther 2010;125:169-79.
- Misawa F, Shimizu K, Fujii Y, Miyata R, Koshiishi F, Kobayashi M, et al. Is antipsychotic polypharmacy associated with metabolic syndrome even after adjustment for lifestyle effects? A cross-sectional study. BMC Psychiatry 2011;11:118.
- Essock SM, Schooler NR, Stroup TS, McEvoy JP, Rojas I, Jackson C, et al. Effectiveness of switching from antipsychotic polypharmacy to monotherapy. Am J Psychiatry 2011;168:702-8.
- Mackin P, Watkinson HM, Young AH. Prevalence of obesity, glucose homeostasis disorders and metabolic syndrome in psychiatric patients taking typical or atypical antipsychotic drugs: a cross-sectional study. Diabetologia 2005;48:215-21.
- Hägg S, Joelsson L, Mjörndal T, Spigset O, Oja G, Dahlqvist R. Prevalence of diabetes and impaired glucose tolerance in patients treated with clozapine compared with patients treated with conventional depot neuroleptic medications. J Clin Psychiatry 1998;59:294-9.
- Alberti KG, Zimmet P, Shaw J. Metabolic syndrome — a new world-wide definition. A Consensus Statement from the International Diabetes Federation. Diabet Med 2006;23:469-80.
- Alberti KG, Zimmet PZ. Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: Diagnosis and classification of diabetes mellitus, provisional report of a WHO commission. Diabet Med 1998;15:539-53.
- Balkau B, Charles MA. Comment on the provisional report from the WHO consultation. European Group for the Study of Insulin Resistance (EGIR). Diabet Med 1999;16:442-3.
- Bloomgarden ZT. American Diabetes Association Annual Meeting, June 2003. Gastrointestinal and dietary aspects of diabetes. Diabetes Care 2003;26:2941-6.
- Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive Summary of The Third Report of The National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, And Treatment of High Blood Cholesterol In Adults (Adult Treatment Panel III). JAMA 2001;285:2486-97.
- Wildman RP, Gu D, Reynolds K, Duan X, He J. Appropriate body mass index and waist circumference cutoffs for categorization of overweight and central adiposity among Chinese adults. Am J Clin Nutr 2004;80:1129-36.
- Ford ES, Giles WH, Dietz WH. Prevalence of the metabolic syndrome among US adults: findings from the third National Health and Nutrition Examination Survey. JAMA 2002;287:356-9.
- Hoang KC, Le TV, Wong ND. The metabolic syndrome in East Asians. J Cardiometab Syndr 2007;2:276-82.
- Hu G, Lindström J, Jousilahti P, Peltonen M, Sjöberg L, Kaaja R, et al. The increasing prevalence of metabolic syndrome among Finnish men and women over a decade. J Clin Endocrinol Metab 2008;93:832-6.
- McEvoy JP, Meyer JM, Goff DC, Nasrallah HA, Davis SM, Sullivan L, et al. Prevalence of the metabolic syndrome in patients with schizophrenia: baseline results from the Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) schizophrenia trial and comparison with national estimates from NHANES III. Schizophr Res 2005;80:19-32.
- Goossens GH. The role of adipose tissue dysfunction in the pathogenesis of obesity-related insulin resistance. Physiol Behav 2008;94:206-18.
- Scheen AJ, De Hert MA. Abnormal glucose metabolism in patients treated with antipsychotics. Diabetes Metab 2007;33:169-75.
- Kohen D. Diabetes mellitus and schizophrenia: historical perspective. Br J Psychiatry Suppl 2004;47:S64-6.
- Grundy SM. Hypertriglyceridemia, insulin resistance, and the metabolic syndrome. Am J Cardiol 1999;83:25F-29F.
- van Winkel R, van Os J, Celic I, Van Eyck D, Wampers M, Scheen A, et al. Psychiatric diagnosis as an independent risk factor for metabolic disturbances: results from a comprehensive, naturalistic screening program. J Clin Psychiatry 2008;69:1319-27.
- Watanabe H, Tanabe N, Watanabe T, Darbar D, Roden DM, Sasaki S, et al. Metabolic syndrome and risk of development of atrial fibrillation: the Niigata preventive medicine study. Circulation 2008;117:1255-60.
- Kotronen A, Yki-Järvinen H. Fatty liver: a novel component of the metabolic syndrome. Arterioscler Thromb Vasc Biol 2008;28:27-38.
- Goldbacher EM, Matthews KA. Are psychological characteristics related to risk of the metabolic syndrome? A review of the literature. Ann Behav Med 2007;34:240-52.
- Welzel TM, Graubard BI, Zeuzem S, El-Serag HB, Davila JA, McGlynn KA. Metabolic syndrome increases the risk of primary liver cancer in the United States: a study in the SEER-Medicare database. Hepatology 2011;54:463-71.
- Gottlieb AB, Dann F, Menter A. Psoriasis and the metabolic syndrome. J Drugs Dermatol 2008;7:563-72.
- De Hert M, Dobbelaere M, Sheridan EM, Cohen D, Correll CU. Metabolic and endocrine adverse effects of second-generation antipsychotics in children and adolescents: a systematic review of randomized, placebo controlled trials and guidelines for clinical practice. Eur Psychiatry 2011;26:144-58.
- Yau PL, Castro MG, Tagani A, Tsui WH, Convit A. Obesity and metabolic syndrome and functional and structural brain impairments in adolescence. Pediatrics 2012;130:e856-64.
- Simon V, van Winkel R, De Hert M. Are weight gain and metabolic side effects of atypical antipsychotics dose dependent? A literature review. J Clin Psychiatry 2009;70:1041-50.
- Allison DB, Fontaine KR, Heo M, Mentore JL, Cappelleri JC, Chandler LP, et al. The distribution of body mass index among individuals with and without schizophrenia. J Clin Psychiatry 1999;60:215-20.
- Thakore JH, Mann JN, Vlahos I, Martin A, Reznek R. Increased visceral fat distribution in drug-naive and drug-free patients with schizophrenia. Int J Obes Relat Metab Disord 2002;26:137-41.
- Tschoner A, Engl J, Laimer M, Kaser S, Rettenbacher M, Fleischhacker WW, et al. Metabolic side effects of antipsychotic medication. Int J Clin Pract 2007;61:1356-70.
- Allison DB, Casey DE. Antipsychotic-induced weight gain: a review of the literature. J Clin Psychiatry 2001;62 Suppl 7:S22-31.
- McIntyre RS, Mancini DA, Basile VS. Mechanisms of antipsychotic- induced weight gain. J Clin Psychiatry 2001;62 Suppl 23:S23-9.
- Llorente MD, Urrutia V. Diabetes, psychiatric disorders, and the metabolic effects of antipsychotic medications. Clin Diabetes 2006;24:18-24.
- Taylor D, Paton C, Kerwin R. The Maudsley prescribing guidelines. 9th ed. London, Routledge; 2007.
- Hasnain M, Fredrickson SK, Vieweg WV, Pandurangi AK. Metabolic syndrome associated with schizophrenia and atypical antipsychotics. Curr Diab Rep 2010;10:209-16.
- Clark NG. Consensus development conference on antipsychotic drugs and obesity and diabetes. Diabetes Care 2004;27:596-601.
- Zhang XY, Zhou DF, Wu GY, Cao LY, Tan YL, Haile CN, et al. BDNF levels and genotype are associated with antipsychotic-induced weight gain in patients with chronic schizophrenia. Neuropsychopharmacology 2008;33:2200-5.
- Dixon L, Weiden P, Delahanty J, Goldberg R, Postrado L, Lucksted A, et al. Prevalence and correlates of diabetes in national schizophrenia samples. Schizophr Bull 2000;26:903-12.
- Perkins DO. Predictors of noncompliance in patients with schizophrenia. J Clin Psychiatry 2002;63:1121-8.
- Koro CE, Fedder DO, L’Italien GJ, Weiss SS, Magder LS, Kreyenbuhl J, et al. Assessment of independent effect of olanzapine and risperidone on risk of diabetes among patients with schizophrenia: population- based nested case-control study. BMJ 2002;325:243-7.
- Sernyak MJ, Leslie DL, Alarcon RD, Losonczy MF, Rosenheck R. Association of diabetes mellitus with use of atypical neuroleptics in the treatment of schizophrenia. Am J Psychiatry 2002;159:561-6.
- Reinstein MJ, Sirotovskaya LA, Jones LE, Mohan S, Chasanov MA. Effect of clozapine-quetiapine combination therapy on weight and glycaemic control: preliminary findings. Clin Drug Investig 1999;18:99-104.
- Campanella LM, Lartey R, Shih R. Severe hyperglycemic hyperosmolar nonketotic coma in a nondiabetic patient receiving aripiprazole. Am Emerg Med 2009;53:264-6.
- Baldessarini RJ, Lipinski JF. Toxicity and side-effects of antipsychotic, antimanic, and antidepressant medications. Psychiatr Ann 1976;6:52-68.
- Baptista T, Lacruz A, Angeles F, Silvera R, de Mendoza S, Mendoza MT, et al. Endocrine and metabolic abnormalities involved in obesity associated with typical antipsychotic drug administration. Pharmacopsychiatry 2001;34:223-31.
- Smith M, Hopkins D, Peveler RC, Holt RI, Woodward M, Ismail K. First- v. second-generation antipsychotics and risk for diabetes in schizophrenia: systematic review and meta-analysis. Br J Psychiatry 2008;192:406-11.
- Johnson DE, Yamazaki H, Ward KM, Schmidt AW, Lebel WS, Treadway JL, et al. Inhibitory effects of antipsychotics on carbachol- enhanced insulin secretion from perifused rat islets: role of muscarinic antagonism in antipsychotic-induced diabetes and hyperglycemia. Diabetes 2005;54:1552-8.
- Buchholz S, Morrow AF, Coleman PL. Atypical antipsychotic- induced diabetes mellitus: an update on epidemiology and postulated mechanisms. Intern Med J 2008;38:602-6.
- Sasaki J, Funakoshi M, Arakawa K. Lipids and apolipoproteins in patients treated with major tranquilizers. Clin Pharmacol Ther 1985;37:684-7.
- Lieberman JA, Stroup TS, McEvoy JP, Swartz MS, Rosenheck RA, Perkins DO, et al. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia. N Engl J Med 2005;353:1209-23.
- Spivak B, Roitman S, Vered Y, Mester R, Graff E, Talmon Y, et al. Diminished suicidal and aggressive behavior, high plasma norepinephrine levels, and serum triglyceride levels in chronic neuroleptic-resistant schizophrenic patients maintained on clozapine. Clin Neuropharmacol 1998;21:245-50.
- De Hert M, Hanssens L, van Winkel R, Wampers M, Van Eyck D, Scheen A, et al. A case series: evaluation of the metabolic safety of aripiprazole. Schizophr Bull 2007;33:823-30.
- Cohn T, Prud’homme D, Streiner D, Kameh H, Remington G. >Characterizing coronary heart disease risk in chronic schizophrenia: high prevalence of the metabolic syndrome. Can J Psychiatry 2004;49:753-60.
- Zipursky RB, Gu H, Green AI, Perkins DO, Tohen MF, McEvoy JP, et al. Course and predictors of weight gain in people with first-episode psychosis treated with olanzapine or haloperidol. Br J Psychiatry 2005;187:537-43.
- Rummel-Kluge C, Komossa K, Schwarz S, Hunger H, Schmid F, Lobos CA, et al. Head-to-head comparisons of metabolic side effects of second generation antipsychotics in the treatment of schizophrenia: a systematic review and meta-analysis. Schizophr Res 2010;123:225-33.
- Melkersson KI, Dahl ML, Hulting AL. Guidelines for prevention and treatment of adverse effects of antipsychotic drugs on glucose- insulin homeostasis and lipid metabolism. Psychopharmacology (Berl) 2004;175:1-6.
- Li Z, Maglione M, Tu W, Mojica W, Arterburn D, Shugarman LR, et al. Meta-analysis: pharmacologic treatment of obesity. Ann Intern Med 2005;142:532-46.